With vascular neurologist near me at the forefront, you’re taking the first step towards receiving top-notch medical care for your vascular-related concerns. As a highly specialized field of medicine, vascular neurology focuses on the diagnosis and treatment of conditions affecting the blood vessels in your brain, including stroke, brain aneurysm, and cerebral vasculitis. By consulting a vascular neurologist near you, you can expect expert guidance and treatment options tailored to your specific needs.
The significance of vascular neurology cannot be overstated, as the timely intervention of a vascular neurologist can significantly improve patient outcomes and reduce the risk of long-term damage. By working closely with a vascular neurologist near you, you can navigate the complexities of vascular-related conditions with confidence, knowing you’re under the care of a medical expert dedicated to helping you regain optimal health.
Understanding the Role of a Vascular Neurologist in Modern Healthcare: Vascular Neurologist Near Me
Vascular neurologists play a critical role in modern healthcare, particularly in the treatment and management of stroke and related conditions. These medical professionals specialize in diagnosing and treating disorders of the brain, spinal cord, and their blood vessels, making them essential to the care of patients with vascular-related neurological issues.
The Significance of Vascular Neurology in Treating Stroke and Related Conditions
Vascular neurology is a field of medicine that focuses on the diagnosis, treatment, and prevention of disorders affecting the brain and its blood vessels. These disorders can be caused by a variety of factors, including high blood pressure, atherosclerosis, and blood clots. Vascular neurologists are trained to recognize and treat these conditions promptly, often at the onset of symptoms.
Vascular neurologists diagnose and manage a range of conditions, including:
- Transient ischemic attack (TIA) or ‘mini-stroke.’
- Stroke caused by an ischemic (blood flow obstruction) or hemorrhagic (bleeding) event.
- Carotid artery disease and other arterial conditions affecting the neck and head.
- Cerebral vasculitis and other inflammatory conditions affecting the blood vessels.
Diagnosing Vascular Disorders
Vascular neurologists use a combination of imaging studies and physical examination to diagnose vascular disorders. These imaging studies include:
- Computed Tomography (CT) scans and magnetic resonance imaging (MRI) to visualize the brain and its blood vessels.
- Carotid Doppler ultrasonography to assess blood flow in the neck arteries.
- Angiography to visualize the blood vessels and identify blockages or damage.
Managing Vascular Disorders
Once a diagnosis is made, vascular neurologists develop a treatment plan to manage the condition. This plan may include:
- Medications to control high blood pressure, prevent stroke, or dissolve blood clots.
- Surgical procedures, such as carotid endarterectomy, to remove blockages or plaque from the arteries.
- Interventional radiology procedures, such as angioplasty and stenting, to improve blood flow and prevent further damage.
By understanding the role of vascular neurologists in modern healthcare, patients can seek timely and effective treatment for vascular-related neurological conditions, improving their quality of life and reducing the risk of complications and long-term damage.
Vascular Neurology Services
A vascular neurologist provides comprehensive care for patients with vascular disorders affecting the brain and nervous system. These services include diagnosis, treatment options, and patient care. Vascular neurologists use a multidisciplinary approach to manage a wide range of conditions, from stroke and transient ischemic attack (TIA) to cerebral amyloid angiopathy and spinal vascular malformations.
Vascular neurologists offer various services to diagnose and manage vascular disorders. These services may include:
- Imaging studies such as magnetic resonance imaging (MRI) and computed tomography (CT) scans to evaluate the brain and blood vessels
- Electrophysiological tests like electroencephalography (EEG) and electromyography (EMG) to assess nerve function
- Non-invasive vascular studies like ultrasound and Doppler ultrasonography to assess blood flow and vascular function
- Diagnostic angiography to visualize the blood vessels and assess for blockages or malformations
- Genetic testing to identify genetic defects associated with vascular disorders
Vascular neurologists employ various treatment options to address vascular disorders. These options may include:
- Medications to reduce blood pressure, prevent blood clots, or manage symptoms like pain and fatigue
- Therapeutic angioplasty and stenting to open up blocked blood vessels
- Revascularization surgery to repair or bypass damaged blood vessels
- Aneurysm clipping or coiling to prevent rupture
- Tumor embolization to block blood flow to certain tumors
- Spinal cord stimulation to manage chronic pain and improve function
Advantages and Disadvantages of Treatment Approaches for Vascular Disorders
Comparing Treatment Options
The choice of treatment for vascular disorders depends on several factors, including the underlying cause of the condition, the patient’s overall health, and the severity of symptoms. Two common treatment approaches are endovascular therapy and open surgery.
| | Endovascular Therapy | Open Surgery |
|—|————————-|———————-|
| | Advantage | Advantage |
| 1 | Minimally invasive | Direct access to blockages|
| | No incision or scarring | Can address complex cases |
| | Quicker recovery time | More effective for certain conditions |
| | Reduced risk of bleeding| | |
| | | |
| | Disadvantage | Disadvantage |
| 1 | May not be suitable for all cases | More invasive |
| | Higher risk of complications | Risk of infection |
| | May require multiple sessions | Longer recovery time |
| | | |
In conclusion, vascular neurologists provide comprehensive care for patients with vascular disorders, utilizing a range of diagnostic and treatment options. Understanding the advantages and disadvantages of different treatment approaches is crucial in making informed decisions about managing vascular disorders.
Preparing for a Consultation with a Vascular Neurologist
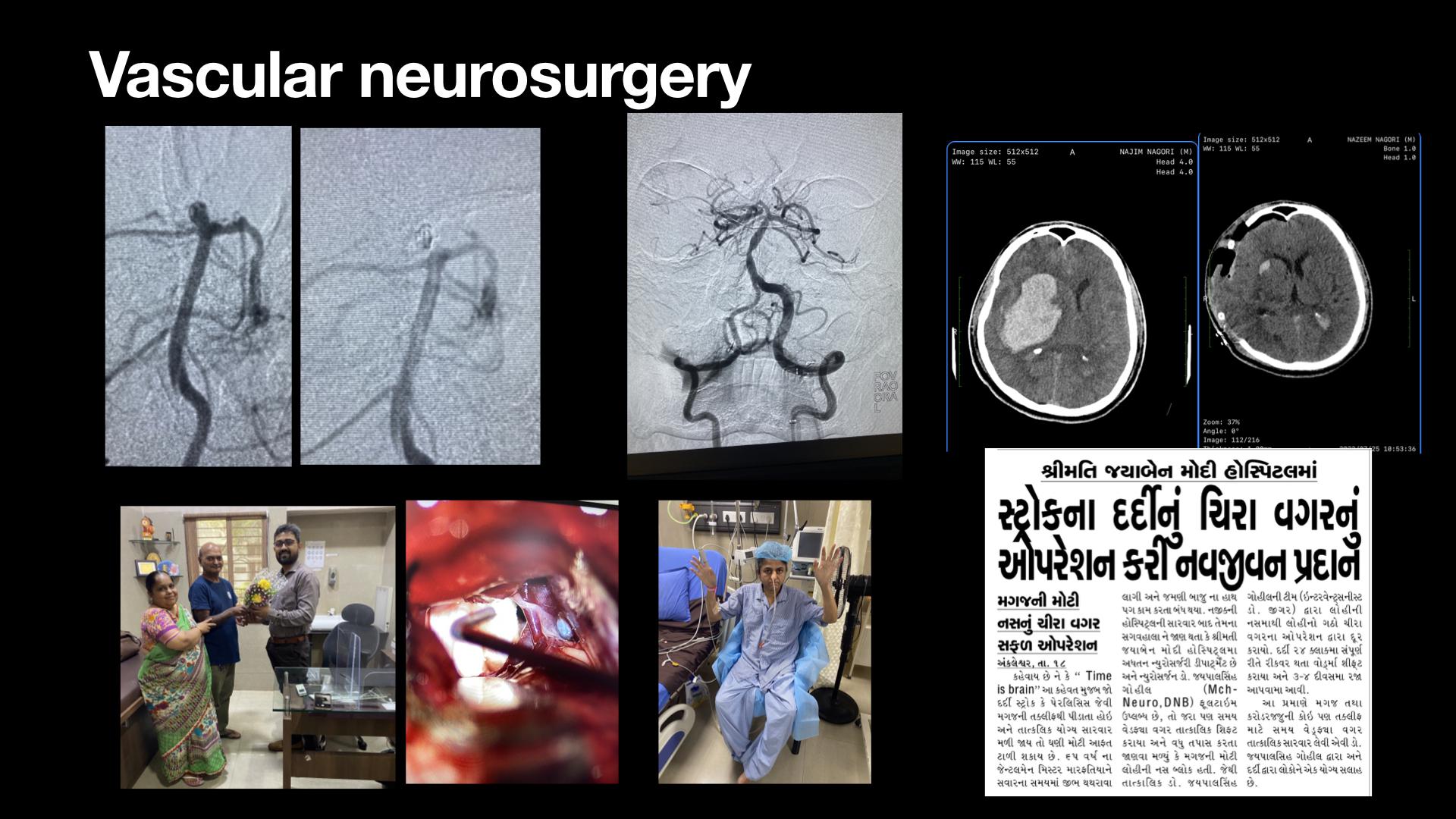
A consultation with a vascular neurologist is a valuable opportunity to discuss your concerns and receive expert advice on managing vascular-related conditions. To make the most out of this consultation, it’s essential to be well-prepared and knowledgeable about the topic. This section will guide you on how to prepare for a consultation with a vascular neurologist, including questions to ask, and the importance of a medical history.
Importance of a Medical History in Your Initial Consultation
A medical history is a critical component of your initial consultation with a vascular neurologist. This includes information about your past medical conditions, family medical history, allergies, and current medications. A detailed medical history allows your vascular neurologist to understand your overall health and identify potential risk factors for vascular-related conditions. It also enables your vascular neurologist to develop an accurate diagnosis and create an effective treatment plan tailored to your specific needs.
When sharing your medical history, be sure to include information about your:
* Past medical conditions, including any hospitalizations or surgeries
* Family medical history, including any relatives with vascular-related conditions
* Current medications, including any supplements or herbal remedies
* Allergies, including any reactions to medications or foods
* Lifestyle habits, including diet, exercise, and smoking history
Questions to Ask Your Vascular Neurologist During a Consultation
During your consultation with a vascular neurologist, it’s essential to ask questions to clarify your diagnosis, treatment plan, and any concerns you may have. Here are some examples of questions to ask your vascular neurologist:
* What are the latest procedures available for treating vascular-related conditions?
* What are the potential side effects of my medication, and how can I manage them?
* How often should I follow up with you for check-ups and appointments?
* Are there any lifestyle changes I can make to reduce my risk of developing vascular-related conditions?
* What are the chances of my symptoms being related to a rare condition?
What to Expect During Your Consultation
During your consultation, your vascular neurologist will conduct a thorough examination, including a physical exam, medical history, and may order diagnostic tests such as imaging studies or blood work. Based on the results, they will discuss your diagnosis, treatment options, and recommend a course of action. Be sure to ask questions and clarify any concerns you may have during this time.
Vascular Neurology Treatments and Procedures

Vascular neurologists use various treatments and procedures to diagnose and manage vascular disorders affecting the brain and nervous system. These treatments aim to improve blood flow, prevent further damage, and promote healing.
Microvascular Bypass Surgery
Microvascular bypass surgery is a complex procedure used to bypass blocked or narrowed blood vessels in the brain. During this surgery, a vascular neurosurgeon or neurointerventionalist creates a detour, or bypass, using a graft from the patient’s own blood vessel or an artificial material. This bypass allows blood to flow around the blockage, reducing pressure on surrounding brain tissue.
The benefits of microvascular bypass surgery include improved blood flow, reduced risk of stroke, and potentially, improved symptoms. However, this surgery is typically reserved for complex cases where other treatments have failed or are not suitable.
Endovascular Intervention
Endovascular intervention, also known as minimally invasive therapy, involves the use of a catheter to deliver a small device or medication directly to the affected blood vessel. Vascular neurologists may use endovascular intervention to:
– Remove blood clots causing strokes or transient ischemic attacks (TIAs)
– Deploy stents or balloon angioplasty to widen narrowed blood vessels
– Place coils or other devices to stop bleeding or embolization
This minimally invasive approach reduces recovery time and minimizes tissue damage compared to traditional open surgery.
Minimally Invasive Treatment Options: Angioplasty and Thrombolysis
Angioplasty and thrombolysis are two commonly used minimally invasive treatments for vascular disorders.
Angioplasty involves using a balloon to widen narrowed or blocked blood vessels. A small catheter is inserted into the affected vessel, and a balloon is inflated to push against the wall of the vessel, restoring blood flow.
Thrombolysis involves using medication to dissolve blood clots. Vascular neurologists may administer tPA (tissue plasminogen activator) or other thrombolytic agents directly into the affected blood vessel or systemically to dissolve blood clots.
Both angioplasty and thrombolysis are used to quickly restore blood flow and reduce the risk of further complications.
Comparison of Minimally Invasive Treatment Options
The choice between angioplasty and thrombolysis depends on the specific vascular disorder and the individual patient’s needs. Vascular neurologists consider factors such as the location, severity, and cause of the blockage or clot when selecting the most appropriate treatment.
In some cases, angioplasty may be more effective for long-term blood flow restoration. However, thrombolysis may be a better option for rapidly dissolving blood clots and restoring blood flow in emergency situations.
-
– Angioplasty is often used for narrowed or occluded blood vessels caused by atherosclerosis, while thrombolysis is typically used for acute ischemic stroke caused by a blood clot.
– Both treatments can be performed under general anesthesia or conscious sedation, and recovery times vary depending on the individual and the treatment used.
– Vascular neurologists closely monitor patients undergoing these procedures to ensure safe and effective treatment.
Navigating the Healthcare System as a Vascular Neurology Patient
As a vascular neurology patient, I can attest to the importance of good patient care in managing chronic conditions. My grandmother’s experience with a vascular neurologist comes to mind. She was diagnosed with a stroke and required ongoing treatment to prevent further complications. Her vascular neurologist took the time to educate her and her family about her condition, its symptoms, and her treatment options. This open communication allowed them to make informed decisions about her care, and as a result, she was able to manage her condition effectively and lead a fulfilling life.
Open communication between patients, vascular neurologists, and other healthcare professionals is crucial in achieving successful treatment outcomes. When patients feel comfortable sharing their concerns and questions with their healthcare providers, they are more likely to adhere to their treatment plans and achieve optimal results. Vascular neurologists, in particular, play a vital role in coordinating care for patients with complex vascular conditions, often requiring the input of multiple specialists. By fostering a collaborative and patient-centered approach, vascular neurologists can ensure that their patients receive comprehensive and coordinated care.
The Importance of Coordination of Care
In vascular neurology, coordination of care is a critical aspect of patient management. Patients often require treatments and interventions from various specialists, including cardiologists, radiologists, and neurosurgeons. A vascular neurologist must navigate this complex network of healthcare professionals to ensure that each specialist is aware of the patient’s treatment plan and any necessary precautions or medications.
- Regularly scheduled appointments with the vascular neurologist and other specialists to ensure everyone is on the same page.
- Clear and concise communication about the patient’s condition, treatment plan, and any medication-related concerns.
- Collaborative decision-making between healthcare professionals and the patient to ensure all parties are aware of the patient’s needs and preferences.
Empowering Patients through Education
Empowering patients with accurate and relevant information about their condition is essential for effective management. Vascular neurologists can educate patients about their treatments, including medications, lifestyle modifications, and potential complications. This education enables patients to make informed decisions about their care, participate actively in their treatment plans, and take ownership of their health.
- Understanding the patient’s condition, its symptoms, and potential complications.
- Familiarity with the patient’s treatment plan, including medications, dosages, and side effects.
- Knowledge of lifestyle modifications that can help prevent or manage vascular conditions.
Addressing Barriers to Care
Patients may encounter various barriers to accessing appropriate care, including accessibility, cost, and communication challenges. Vascular neurologists can play a crucial role in addressing these barriers by providing personalized care, coordinating referrals to specialized services, and advocating for patient needs.
- Addressing language or cultural barriers to ensure effective communication.
- Connecting patients with resources and support services to facilitate access to care.
- Communicating with patients about treatment options and potential costs to ensure informed decision-making.
Staying Up-to-Date with the Latest Advances in Vascular Neurology

As a vascular neurologist, staying current with the latest advances in the field is crucial to delivering the best possible care to patients. The field of vascular neurology is rapidly evolving, with new treatments, technologies, and research emerging regularly. In this section, we will explore the importance of staying up-to-date with the latest advances in vascular neurology and how it impacts clinical practice and patient outcomes.
Importance of Staying Up-to-Date
Staying current with the latest advances in vascular neurology is essential for several reasons. Firstly, new treatments and technologies are continually being developed and introduced into clinical practice. For instance, advancements in thrombectomy devices have improved outcomes for patients with acute ischemic stroke. Secondly, research in vascular neurology is continually evolving, with new trials and studies emerging regularly. This includes studies on novel biomarkers for hemorrhagic stroke and new therapeutic targets for cerebral vasculitis. By staying up-to-date with the latest research and developments, vascular neurologists can provide the most effective treatments and make informed decisions about patient care.
Evaluation of Research Studies, Vascular neurologist near me
To evaluate the effectiveness of different research studies examining novel treatments for vascular disorders, let’s consider the following table:
| Study | Treatment | Outcome Measures | Effectiveness |
|---|---|---|---|
| Study A | Tissue plasminogen activator (tPA) | Recanalization success rate, neurological outcome scores | 80% recanalization success rate, significant improvement in neurological outcomes |
| Study B | Vitamin K antagonists | Stroke recurrence rates, all-cause mortality | 30% stroke recurrence rate, 10% all-cause mortality |
| Study C | Endovascular thrombectomy (EVT) | Recanalization success rate, modified Rankin Scale (mRS) scores | 90% recanalization success rate, improved mRS scores in 70% of patients |
Impact on Clinical Practice and Patient Outcomes
The latest research in vascular neurology has a significant impact on clinical practice and patient outcomes. For example, the use of thrombectomy devices has improved outcomes for patients with acute ischemic stroke by restoring blood flow to the brain in a timely manner. Additionally, studies on novel biomarkers for hemorrhagic stroke have allowed for earlier diagnosis and treatment of patients, leading to improved outcomes. Furthermore, research on new therapeutic targets for cerebral vasculitis has led to the development of more effective treatments for this condition.
The latest research in vascular neurology has also led to the development of new treatments and technologies. For instance, the use of MRI imaging has improved diagnostic accuracy and allowed for earlier identification of vascular disorders. Additionally, the use of artificial intelligence and machine learning algorithms has improved the prediction of stroke risk and identification of high-risk patients.
Summary
Navigating the healthcare system can be overwhelming, but with a vascular neurologist near me, you’ll have a trusted partner guiding you every step of the way. By building a strong relationship with your vascular neurologist and staying informed about the latest advances in vascular neurology, you can take control of your vascular-related health concerns and achieve the best possible outcomes.
Clarifying Questions
What is the primary focus of a vascular neurologist’s practice?
A vascular neurologist’s primary focus is on the diagnosis and treatment of conditions affecting the blood vessels in the brain, including stroke, brain aneurysm, cerebral vasculitis, and blood vessel disease.
How do I locate a vascular neurologist near me?
There are several ways to find a vascular neurologist near you, including searching online directories, asking for referrals from your primary care physician, or consulting with your insurance provider.
What should I expect during a consultation with a vascular neurologist?
During a consultation with a vascular neurologist, you can expect to discuss your symptoms, medical history, and any concerns you may have. Your vascular neurologist will also perform a physical examination and order diagnostic tests as needed to determine the best course of treatment.
How can I build a strong relationship with my vascular neurologist?
To build a strong relationship with your vascular neurologist, be open and honest about your symptoms and concerns. Ask questions, and don’t hesitate to seek a second opinion if you’re unsure about your diagnosis or treatment plan.