Tilt table test near me sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail with exclusive interview style and brimming with originality from the outset. As we delve into the world of medical diagnostics, it becomes clear that tilt table tests have emerged as a vital tool in the quest to understand and manage conditions related to autonomic nervous system dysfunction.
But what exactly is tilt table testing, and why has it become such an essential diagnostic tool? To answer this question, we must delve into the history of tilt table testing, its effectiveness in diagnosing a range of conditions, and the key factors involved in the testing process.
How to Prepare for a Tilt Table Test near Me
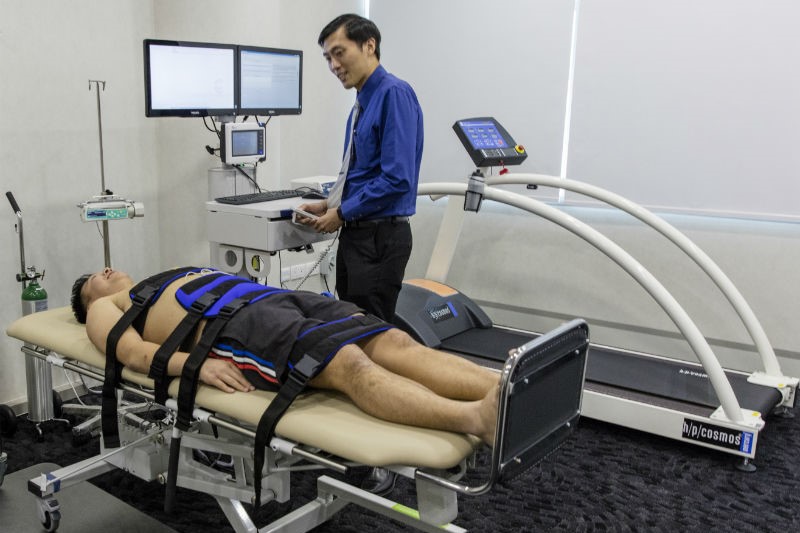
A tilt table test, also known as a head-up tilt table test or HUTT, is a medical procedure used to diagnose various conditions related to the autonomic nervous system, including syncope, orthostatic hypotension, and postural orthostatic tachycardia syndrome (POTS). To ensure a smooth and accurate test, it is essential to prepare adequately before the procedure. This guide provides step-by-step instructions for patients to prepare for a tilt table test.
Pre-Test Preparation
Preparation for the tilt table test involves some adjustments to your daily routine, including medication restrictions, fasting, and avoiding certain activities.
- Medication Restrictions: Inform your doctor about all the medications, vitamins, and supplements you are taking. Some medications may need to be discontinued or adjusted before the test.
- Fasting: Your doctor may ask you to fast for 4-6 hours before the test. This is to ensure that your stomach is empty during the procedure, reducing the risk of nausea and vomiting.
- Avoid Certain Activities: Avoid heavy exercise, hot showers, or baths for 24 hours before the test. These activities can cause your body temperature to rise, potentially affecting the test results.
- Dress Code: Wear loose, comfortable clothing, preferably in layers. This will allow your technician to easily attach the ECG electrodes and other monitoring equipment.
Patient Education and Informed Consent
Patient education is a crucial aspect of the tilt table test process. It’s essential to inform patients about the procedure, potential risks, and expected outcomes.
- Understand the Purpose: The tilt table test is used to diagnose and evaluate the response of the autonomic nervous system to changes in blood pressure and heart rate.
- Expected Outcomes: The test may cause dizziness, lightheadedness, or nausea. In rare cases, patients may experience syncope or other serious complications.
- Risks and Complications: Patients with certain medical conditions, such as pacemakers or other implanted devices, may need to inform their doctor before the test.
Scheduling and Coordinating the Test
Scheduling and coordinating the tilt table test requires careful planning and coordination with your healthcare provider.
- Contact Your Doctor: Schedule an appointment with your doctor to discuss your eligibility for the test and any necessary preparation.
- Test Duration: The test typically takes 30-60 minutes to complete. You will be asked to lie on the tilt table and remain still for the duration of the test.
- Test Results: Your doctor will review the test results with you and discuss the implications for your diagnosis and treatment.
Managing Anxiety and Fear
It’s normal to feel anxious or fearful about the tilt table test, but there are ways to manage these emotions and ensure a smooth experience.
- Communicate with Your Doctor: Inform your doctor about your concerns and ask questions about the test.
- Relaxation Techniques: Practice relaxation techniques, such as deep breathing, progressive muscle relaxation, or meditation, to help manage anxiety.
- Support System: Bring a trusted family member or friend to provide emotional support during the test.
Tilt Table Test Methods and Procedures Explained
The tilt table test is a medical procedure used to diagnose and evaluate various conditions, including postural orthostatic tachycardia syndrome (POTS), neurocardiogenic syncope, and vasovagal syncope. The test involves tilting the patient’s body to different positions to observe their autonomic nervous system’s response to gravity.
Components Involved in Conducting a Tilt Table Test
A tilt table test typically involves several key components:
- The tilt table: This is the primary equipment used in the test. It consists of a flat surface that can be tilted to various angles, allowing the patient to be placed in different positions.
- The electrocardiogram (ECG) monitoring system: The ECG monitors the patient’s heart rate and rhythm during the test, providing crucial information about the heart’s response to tilting.
- The blood pressure measurement system: This system measures the patient’s blood pressure at regular intervals during the test, helping to assess their cardiovascular response.
- The oxygen saturation monitor: This monitor tracks the patient’s oxygen levels in their blood, ensuring that they remain within a safe range during the test.
The combination of these components allows clinicians to gather a comprehensive understanding of the patient’s physiological response to positional changes, thereby aiding in the diagnosis and management of various conditions.
Different Types of Tilt Table Tests
There are two primary types of tilt table tests: active and passive testing.
- Active testing: In this type of test, the patient is actively engaged in physical activity while being tilted. For example, they might be asked to walk or jog on a treadmill while being tilted to different angles. Active testing is often used to assess the patient’s autonomic nervous system’s response to exercise and gravitational stress.
- Passive testing: In passive testing, the patient is not actively engaged in physical activity, and the focus is solely on their physiological response to tilting. Passive testing is often used as a starting point for patients who are unable to tolerate active testing due to symptoms or other medical conditions.
The choice between active and passive testing depends on the patient’s specific needs, medical history, and clinical presentation.
Equipment Used During the Test
In addition to the tilt table, various other pieces of equipment are used during the test to ensure the patient’s safety and comfort:
- Bedside table and accessories: The bedside table holds the ECG monitoring system, blood pressure measurement system, and oxygen saturation monitor, among other equipment. Clinicians use the bedside table to access and adjust the equipment as needed.
- Oxygen supplementation equipment: This equipment provides supplemental oxygen to patients who require additional oxygen during the test. The equipment includes oxygen masks, nasal cannulas, or ventilators.
- Temperature control system: Some tilt tables are equipped with temperature control systems to regulate the patient’s body temperature during the test. This is particularly important for patients with temperature instability or other medical conditions.
The combination of advanced equipment and careful clinical evaluation enables clinicians to conduct a thorough and accurate tilt table test.
Making the Diagnosis: Tilt Table Test Results, Tilt table test near me
The results of a tilt table test are crucial in diagnosing and managing various conditions. Clinicians interpret the test results by analyzing the patient’s autonomic nervous system response to tilting, including changes in heart rate, blood pressure, and oxygen saturation.
Oxford Medical Index lists various criteria for diagnosing tilt-related disorders, including the absence of an adequate heart rate response to a drop in blood pressure.
The accuracy of the test results depends on the patient’s ability to remain still and follow instructions during the procedure. Clinicians use the test results in conjunction with the patient’s medical history, physical examination, and other diagnostic tests to make an accurate diagnosis and develop an effective treatment plan.
Examples of Real-Life Applications
Tilt table tests are commonly used in various medical settings, including:
Research and Clinical Practice
Tilt table tests have been extensively studied and applied in various research and clinical settings to assess the autonomic nervous system’s response to gravitational stress.
According to American College of Cardiology (ACC), tilt table testing has played a significant role in diagnosing POTS in patients.
In conclusion, the tilt table test is a valuable diagnostic tool that provides clinicians with essential information about the autonomic nervous system’s response to gravitational stress.
Tilt Table Test Results and Interpretation
The tilt table test results are crucial in determining the diagnosis and treatment plan for patients suspected of having syncope, orthostatic hypotension, or other orthostatic intolerance disorders. The results of the test provide valuable information about the patient’s autonomic nervous system function, heart rate, and blood pressure responses to orthostatic stress.
Heart Rate Variability and Blood Pressure Variability Analysis
Heart rate and blood pressure variability analysis can provide detailed information about the autonomic nervous system function during the tilt table test. This analysis can help to identify abnormalities in the autonomic nervous system response to orthostatic stress, which can guide treatment decisions and improve patient outcomes.
- High frequency power (HF) is a measure of parasympathetic nervous system activity, which can be decreased in patients with orthostatic intolerance.
- Low frequency power (LF) is a measure of sympathetic nervous system activity, which can be increased in patients with orthostatic intolerance.
- LF/HF ratio is a measure of sympathetic to parasympathetic balance, which can be abnormal in patients with orthostatic intolerance.
Blood Pressure Responses and Orthostatic Hypotension
Blood pressure responses during the tilt table test can provide information about the patient’s ability to maintain blood pressure in the upright position. Orthostatic hypotension is defined as a drop in systolic blood pressure of 20mmHg or more within 3 minutes of standing.
- Mild orthostatic hypotension (drop in systolic blood pressure 10-19mmHg) can be seen in patients with mild autonomic dysfunction.
- Severe orthostatic hypotension (drop in systolic blood pressure 20mmHg or more) is a more severe form of autonomic dysfunction and requires aggressive treatment.
Heart Rate Responses and Postural Tachycardia Syndrome
Heart rate responses during the tilt table test can provide information about the patient’s ability to maintain heart rate in the upright position. Postural tachycardia syndrome (POTS) is defined as an increase in heart rate of 30 beats per minute or more within 10 minutes of standing.
- Mild POTS (heart rate increase 10-29 beats per minute) can be seen in patients with mild autonomic dysfunction.
- Severe POTS (heart rate increase 30 beats per minute or more) is a more severe form of autonomic dysfunction and requires aggressive treatment.
Combining Tilt Table Test Results with Other Diagnostic Tools and Patient-Reported Symptoms
Combining tilt table test results with other diagnostic tools and patient-reported symptoms can provide a more comprehensive picture of the patient’s autonomic nervous system function and orthostatic intolerance. This can guide treatment decisions and improve patient outcomes.
- Heart rate and blood pressure monitoring during exercise stress testing.
- Electrocardiogram (ECG) monitoring during exercise stress testing.
- Autonomic nervous system function testing, such as the cold pressor test.
- Cardiac output monitoring during exercise stress testing.
- Upright tilt testing with continuous electrocardiogram (ECG) and blood pressure monitoring.
Safety and Risks Associated with Tilt Table Testing

Tilt table testing is a common diagnostic procedure used to evaluate patients with suspected neurocardiogenic syncope or other conditions that affect heart rate and blood pressure regulation. However, like any medical test, there are potential risks and complications associated with tilt table testing. In this section, we will discuss the safety and risks associated with tilt table testing, as well as the measures taken to mitigate these risks and ensure patient safety.
The risks associated with tilt table testing can be divided into several categories, including cardiovascular, neurological, and allergic reactions. Some of the potential risks and complications include vasovagal syncope, hypotension, hypertension, and atrioventricular block. These complications are typically temporary and resolve on their own once the patient is returned to a horizontal position.
Common Complications Associated with Tilt Table Testing
Common complications associated with tilt table testing include:
- Vasovagal syncope: This is the most common complication associated with tilt table testing, occurring in approximately 20-50% of patients. Vasovagal syncope is characterized by a sudden drop in heart rate and blood pressure, which can lead to dizziness, lightheadedness, and even loss of consciousness. This complication is typically resolved once the patient is returned to a horizontal position.
- Hypotension: Hypotension is a common complication associated with tilt table testing, occurring in approximately 10-20% of patients. Hypotension is characterized by a sudden drop in blood pressure, which can lead to dizziness, lightheadedness, and even loss of consciousness. This complication is typically resolved once the patient is returned to a horizontal position.
- Hypertension: Hypertension is a rare complication associated with tilt table testing, occurring in approximately 1-5% of patients. Hypertension is characterized by a sudden increase in blood pressure, which can lead to hypertension, headache, and even stroke. This complication is typically managed with medication and monitoring.
- Atrioventricular block: Atrioventricular block is a rare complication associated with tilt table testing, occurring in approximately 1-5% of patients. Atrioventricular block is characterized by a blockage between the atria and ventricles, which can lead to abnormal heart rhythms and even cardiac arrest. This complication is typically managed with medication and monitoring.
Safety Measures to Mitigate Risks
To mitigate the risks associated with tilt table testing, several safety measures are taken during the procedure. These safety measures include:
- A thorough medical history and physical examination to identify patients at high risk for complications.
- A careful selection of patients for tilt table testing, based on the presence of symptoms and signs associated with neurocardiogenic syncope or other conditions that affect heart rate and blood pressure regulation.
- The use of electrocardiogram (ECG) monitoring to detect any abnormal heart rhythms during the test.
- The use of blood pressure monitoring to detect any sudden changes in blood pressure during the test.
- The use of oxygen therapy to prevent hypoxia in patients with compromised respiratory function.
- The use of medications to prevent or manage complications during the test, such as anticholinergic or vasopressor medications.
Comparison with Other Diagnostic Procedures
Tilt table testing has a relatively low risk profile compared to other diagnostic procedures, such as cardiac catheterization or coronary angiography. However, it is essential to note that tilting table testing is a relatively safe procedure when performed by experienced professionals and with proper monitoring and medical management.
Rare or Unusual Complications
While tilt table testing is generally a safe procedure, there are several rare or unusual complications that can occur. These complications include:
- Hypersensitivity reactions: Rarely, patients may experience hypersensitivity reactions, such as anaphylaxis, during tilt table testing. This complication is typically managed with medication and monitoring.
- Blood clot formation: Rarely, patients may experience blood clot formation during tilt table testing, particularly in patients with pre-existing clotting disorders. This complication is typically managed with medication and monitoring.
- Electrolyte imbalance: Rarely, patients may experience electrolyte imbalances during tilt table testing, particularly in patients with pre-existing electrolyte disorders. This complication is typically managed with medication and monitoring.
Final Wrap-Up

In conclusion, tilt table testing has emerged as a critical diagnostic tool for autonomic nervous system dysfunction, offering valuable insights into the workings of the human body. By understanding the complexities of this diagnostic method, we can better appreciate the importance of accurate diagnosis and treatment, leading to improved outcomes for patients nationwide.
FAQs
Q: What can I expect during a tilt table test?
A: A tilt table test typically involves patients being secured to a table that can be tilted to various positions, while their heart rate, blood pressure, and other vital signs are monitored. This allows healthcare professionals to assess autonomic nervous system function and diagnose conditions such as POTS.
Q: How long does a tilt table test take?
A: The length of a tilt table test can vary depending on the individual and the purpose of the test, but most tests typically last between 45-60 minutes.
Q: Is a tilt table test painful?
A: Tilt table tests are generally considered to be a safe and painless diagnostic tool, but some patients may experience mild discomfort or lightheadedness during or after the test.
Q: Can I eat or drink before a tilt table test?
A: Patients are usually advised to fast for a period of time before undergoing a tilt table test, as certain foods and beverages can affect the test results.
Q: How accurate are tilt table test results?
A: Tilt table test results can be highly accurate when conducted by trained healthcare professionals using standardized procedures and equipment, but results may vary depending on individual factors.