Pediatricians who accept unvaccinated patients near me sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset. The divide between pediatricians who accept unvaccinated patients and those who do not has grown significantly over the years, largely due to cultural and socioeconomic factors.
This gap is not limited to urban areas; rural communities also face challenges in finding accepting pediatricians. As a result, individuals and families are left to navigate a complex and often treacherous landscape in search of healthcare that aligns with their values and needs.
Understanding the Growing Divide between Pediatricians who Accept Unvaccinated Patients and Those who Do Not – Cultural and Socioeconomic Factors: Pediatricians Who Accept Unvaccinated Patients Near Me
In recent years, there has been a growing divide between pediatricians who accept unvaccinated patients and those who do not. This divide is influenced by various cultural and socioeconomic factors that shape pediatricians’ attitudes towards unvaccinated patients. The acceptance or rejection of unvaccinated patients can have significant consequences on the health and well-being of children, especially those who are not yet vaccinated.
Cultural Factors:
Cultural differences play a crucial role in shaping pediatricians’ attitudes towards unvaccinated patients. In some communities, vaccines are viewed with skepticism or distrust, leading to lower vaccination rates. For example, some communities may have limited access to healthcare services or may be exposed to misinformation about vaccine safety and effectiveness. In these cases, pediatricians may struggle to balance their professional obligations with the cultural and social context in which they practice.
Socioeconomic Factors:
Socioeconomic factors also contribute to the divide. Pediatricians who serve low-income or underserved communities may face significant challenges in providing care to unvaccinated patients. These challenges can include limited access to vaccine funding, inadequate storage and handling of vaccines, and difficulty navigating complex healthcare systems. In some cases, pediatricians may be reluctant to see unvaccinated patients due to concerns about the potential risks of vaccine-preventable diseases in their communities.
Real-Life Examples of Cultural and Socioeconomic Factors in Pediatricians’ Attitudes
Cultural Examples
In some communities, parents may choose not to vaccinate their children due to cultural or religious beliefs. For instance, parents from some communities may believe that vaccines contain substances that are considered sacred or forbidden. In these cases, pediatricians may struggle to provide care to unvaccinated patients, as their own cultural or religious beliefs may conflict with the parents’ views. For example, in some African communities, there is a growing concern about vaccine safety, leading to a decrease in vaccination rates.
Socioeconomic Examples
In other cases, pediatricians may be reluctant to take on unvaccinated patients due to socioeconomic concerns. For example, a pediatrician in an urban setting may have limited access to vaccine funding and may struggle to provide care to unvaccinated patients from low-income families. Similarly, a pediatrician in a rural setting may face challenges in accessing vaccines and may be more likely to reject unvaccinated patients due to concerns about the potential risks of vaccine-preventable diseases in their community.
Cases of Pediatricians’ Dilemmas in Unvaccinated Patient Care
Pediatricians often face difficult decisions when caring for unvaccinated patients. These dilemmas can arise when pediatricians must balance their professional obligations with their own personal values and cultural beliefs. In some cases, pediatricians may be required to provide care to unvaccinated patients, even if they personally disagree with the parents’ vaccination decisions. For example, a pediatrician may be required to treat a child with a vaccine-preventable disease, despite the parents’ refusal to vaccinate them.
Challenges in finding pediatricians who accept unvaccinated patients near me – Share personal anecdotes from individuals who have struggled to find accepting pediatricians.

It’s no secret that finding a pediatrician who accepts unvaccinated patients can be a daunting task for many parents. The challenges they face are numerous, and the emotional toll can be high. In this section, we’ll delve into the obstacles and barriers faced by individuals looking for pediatricians who are willing to accept unvaccinated patients. We’ll also compare the experiences of those in urban versus rural areas in terms of access to accepting pediatricians.
Obstacles and Barriers
One of the primary obstacles faced by parents who are seeking pediatricians who accept unvaccinated patients is the lack of transparency in the medical community regarding vaccination policies. Many pediatric offices fail to explicitly state their vaccination requirements, leaving parents to navigate a maze of assumptions and implicit rules. This can lead to feelings of anxiety and uncertainty, as parents try to determine whether their child’s pediatrician will accept their unvaccinated status.
- Communication Breakdown
- Stigma and Judgment
- Urban Areas
- Rural Areas
- Measles: Measles is a highly contagious disease that can be spread through respiratory droplets when an infected person coughs or sneezes. According to the CDC, one person with measles can infect up to 18 other people who are not immune.
- Pertussis (Whooping Cough): Pertussis is a highly contagious disease caused by the bacterium Bordetella pertussis. It can be spread through close contact with an infected person, who may cough or sneeze in the direction of others.
- Influenza: Influenza, commonly known as the flu, is a contagious respiratory illness caused by the influenza virus. It can be spread through droplets when an infected person coughs or sneezes, or through contact with contaminated surfaces.
- Meningococcal Disease: Meningococcal disease is a bacterial infection that can cause meningitis and sepsis. It can be spread through close contact with an infected person, often through sharing utensils, drinks, or other items.
- Lengthy and expensive hospital stays: Patients with severe cases of vaccine-preventable diseases may require prolonged hospitalizations, which can be costly for families and hospitals.
- Intensive care: Patients with severe cases of vaccine-preventable diseases may require intensive care, including life-support machines and antibiotics, which can be expensive.
- Loss of productivity: Families may experience a loss of productivity due to caring for a sick child, which can impact their ability to work and earn a living.
- Understanding the reasons behind vaccine hesitancy, including cultural, social, and personal factors.
- Developing active listening skills to empathize with patients and families, creating a safe and non-judgmental space for discussion.
- Providing accurate and unbiased information about vaccines, addressing common misconceptions and myths.
- Learning how to communicate effectively with unvaccinated patients and families, tailoring their approach to meet the individual needs of each family.
- Developing a non-discriminatory patient selection policy, ensuring equal access to care for all families, regardless of vaccination status.
- Establishing clear communication channels with patients and families, providing them with accurate and timely information about their child’s health and development.
- Implementing flexible appointment scheduling to accommodate patients who may require more time or support during consultations.
- Providing cultural and linguistic services to support families from diverse backgrounds, ensuring they receive equitable care.
- Providing education and resources on the benefits and risks of vaccination, empowering patients and families to make informed decisions.
- Encouraging ongoing dialogue and collaboration with patients and families, addressing their concerns and questions in a non-judgmental and empathetic manner.
- Working with patients and families to develop personalized vaccination plans, considering their individual needs and circumstances.
- Educate patients about the risks and benefits of vaccination, as well as the potential consequences of not vaccinating.
- Explain the community’s collective responsibility in protecting public health and the role that vaccinations play in achieving this goal.
- Offer alternative vaccination schedules or options for patients who have concerns about vaccination safety.
- Maintain open communication with patients about their vaccination status and concerns, while also upholding the Centers for Disease Control and Prevention’s (CDC) vaccination recommendations.
- Collaborate with other healthcare professionals and public health officials to develop local vaccination policies that balance individual patient needs with community protection.
- Allowing patients to choose their vaccination schedule while still adhering to the CDC’s recommended vaccination timeline.
- Offering alternative vaccination products, such as homeopathics, that may address patient concerns while still providing some level of protection against infectious diseases.
- Partnering with patients to develop personalized vaccination plans that address their unique needs and concerns.
- Empowerment through shared experiences
- Access to valuable resources and information
- Expert advice and guidance
- Addressing misconceptions and stigma
- Personal stories of overcoming obstacles
- Valuable resources and recommendations
- Expert insights and guidance
- Online support groups for specific needs
- Be aware of the family’s individual circumstances, such as previous vaccine-related adverse events or cultural or religious concerns.
- Use simple, clear language when discussing vaccination risks and benefits to help parents understand the information.
- Solicit input from parents about their concerns and listen attentively to their perspectives.
- Foster a sense of collaboration by working together to establish goals for vaccination and health.
- Provide parents with accurate, balanced information about vaccination risks and benefits, including the potential consequences of vaccination or non-vaccination.
- Be prepared to address and address concerns about vaccination safety, such as the presence of thimerosal or adjuvants in vaccines.
- Recognize the role of social media and online communities in shaping parents’ perceptions of vaccination risks and benefits.
- Speak in a calm, empathetic tone when discussing vaccine-related concerns or risks.
- Use straightforward language to explain vaccine-related concepts, avoiding technical jargon.
- Ask parents to clarify their questions or concerns to ensure understanding.
- Provide visual aids or handouts with information about vaccine risks and benefits.
- Offer opportunities for follow-up conversations to continue the dialogue on vaccine-related topics.
- Respect parents’ decisions regarding vaccination, even if they differ from the pediatrician’s recommendations.
- Emphasize the importance of vaccination in preventing the spread of vaccine-preventable diseases.
- Discuss potential consequences of non-vaccination, such as outbreaks and increased risk of serious illness.
- Offer support for families who opt for alternative vaccination schedules or options.
- Be approachable and non-judgmental: Maintain a warm and welcoming demeanor, and avoid making assumptions or judgments about a family’s vaccination choices.
- Use clear and simple language: Avoid using technical jargon or complex medical terminology that may confuse or intimidate families.
- Focus on health outcomes: Shift the conversation from vaccination status to overall health outcomes and the importance of regular check-ups and preventive care.
- Respect family values and decisions: Acknowledge and respect families’ choices and values, even if they differ from your own.
- Provide education and resources: Offer families accurate and unbiased information about vaccination risks and benefits, as well as resources to help them make informed decisions.
Parents who choose not to vaccinate their children often report difficulty in finding pediatricians who are willing to communicate openly and honestly about their vaccination policies. This lack of transparency can be especially challenging for parents who are unsure about their child’s health needs or are seeking medical advice.
“I wanted a pediatrician who would listen to me and discuss my concerns about vaccinations. Instead, I found one who seemed to dismiss my questions and simply told me that their office followed the ‘recommended’ vaccination schedule.”
Parents who choose not to vaccinate their children are often met with judgment and stigma from the medical community. Pediatricians may view unvaccinated children as somehow “less healthy” or more “risky” than vaccinated children. This attitude can make it difficult for parents to feel heard and understood, and may lead them to seek medical care from offices that are more accommodating.
In urban areas, the competition for pediatric offices that accept unvaccinated patients can be fierce. Parents may need to navigate long waiting lists or travel long distances to find a pediatrician who is willing to work with their family. Urban areas often have more pediatric offices, but those that do accept unvaccinated patients may be more expensive or harder to schedule appointments with.
In rural areas, the situation is often more dire. There may be fewer pediatric offices available, and those that do exist may be less likely to accept unvaccinated patients. Parents in rural areas may need to travel long distances to access medical care, which can be especially challenging for families with limited mobility or financial resources. The lack of access to pediatric care in rural areas can have serious consequences for children’s health and development.
Comparing Urban and Rural Areas
While both urban and rural areas present challenges for parents seeking pediatricians who accept unvaccinated patients, the experience can be quite different. Urban areas tend to have more pediatric offices available, but those that do accept unvaccinated patients may be more expensive or harder to schedule appointments with. Rural areas, on the other hand, often have fewer options and may require parents to travel long distances to access medical care.
Impacts of Unvaccinated Patients on the Pediatric Healthcare System
The healthcare system is designed to provide care to patients with varying levels of risk, but the presence of unvaccinated individuals can put the entire system at risk. The consequences of widespread unvaccination among children can be severe, not only for the children themselves but also for the hospitals and families affected by the spread of vaccine-preventable diseases.
One of the most significant consequences of widespread unvaccination is the spread of infectious diseases. Children who are not vaccinated are at a higher risk of contracting and spreading diseases such as measles, pertussis, and influenza.
Diseases Spread Through Unvaccinated Patients
Unvaccinated patients can spread vaccine-preventable diseases to other children, who may not have received the necessary vaccinations. This can lead to outbreaks of diseases that were once rare or even eliminated in the United States. Some of the most common diseases spread through unvaccinated patients include:
The financial and emotional burdens of unvaccinated patients on the healthcare system are significant. Hospitals and families may experience increased costs due to:
The economic burden of unvaccinated patients on the healthcare system is significant. According to a study published in the Journal of Infectious Diseases, the annual economic burden of unvaccinated patients in the United States was estimated to be over $10 billion in 2019.
“The spread of vaccine-preventable diseases has a significant economic burden on the healthcare system, families, and society as a whole.” – Centers for Disease Control and Prevention (CDC)
The consequences of widespread unvaccination among children are severe and can have long-lasting impacts on the healthcare system and families. It is essential to increase vaccination rates to protect not only individual children but also the community as a whole.
Creating a Welcoming Environment for Unvaccinated Patients in Pediatrician Offices
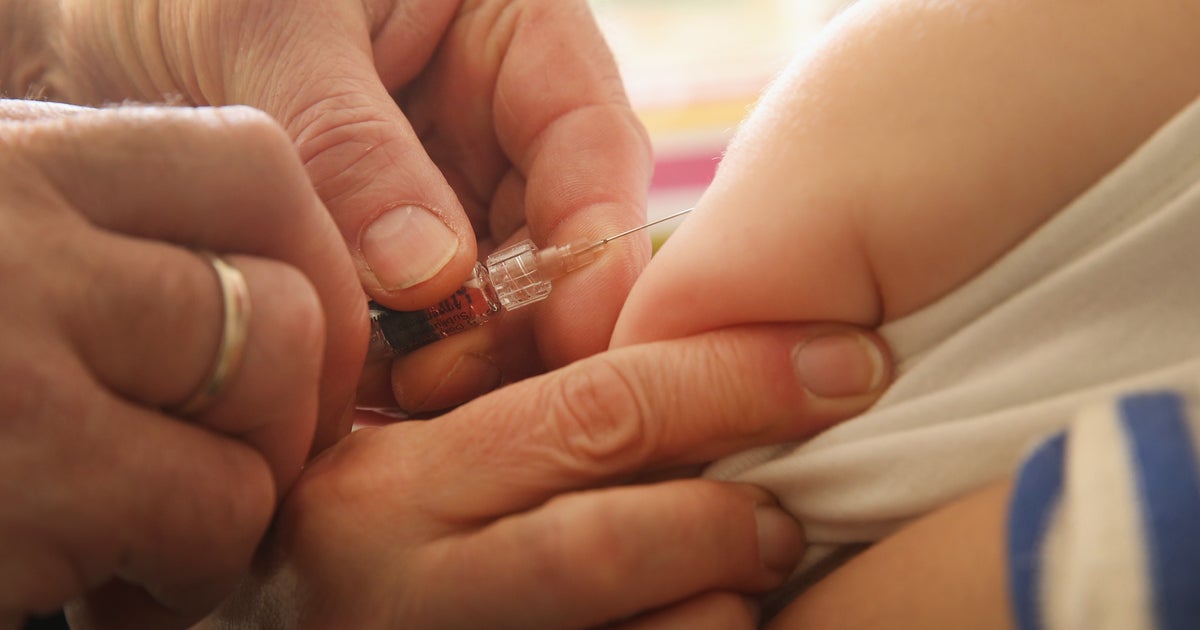
Creating a welcoming environment for unvaccinated patients in pediatrician offices is a crucial step in promoting trust, understanding, and positive health outcomes for these families. By providing a non-judgmental and empathetic space, pediatrician offices can build strong relationships with their patients and families, ultimately leading to better health outcomes and a more collaborative approach to healthcare.
Incorporating a welcoming environment into pediatrician offices can be achieved through various means. Staff training is a vital component, as it equips healthcare professionals with the knowledge and skills necessary to communicate effectively with unvaccinated patients and families. This may involve learning about the reasons behind vaccine hesitancy, active listening skills, and providing accurate and unbiased information.
Staff Training
To create a welcoming environment, pediatrician offices should provide comprehensive staff training to address the unique needs of unvaccinated patients and families. This should include:
Staff training should also involve scenario-based exercises to practice these new skills in a simulated environment, allowing healthcare professionals to feel more confident and prepared in real-life situations.
Policy Revisions, Pediatricians who accept unvaccinated patients near me
To create a welcoming environment, pediatrician offices should also consider revising their policies to accommodate the unique needs of unvaccinated patients and families. This may involve:
By incorporating these policy revisions, pediatrician offices can create a more inclusive and welcoming environment for unvaccinated patients and families, promoting a culture of trust and cooperation.
Balancing Patient Needs with the Importance of Vaccination
Creating a welcoming environment for unvaccinated patients in pediatrician offices requires a delicate balance between accommodating their needs and promoting the importance of vaccination. This can be achieved through:
By walking this fine line, pediatrician offices can create a safe and supportive environment for unvaccinated patients and families, promoting a collaborative approach to healthcare that prioritizes both patient well-being and public health.
Balancing Patient Autonomy with the Responsibility to Protect Public Health
The debate surrounding vaccination policies in pediatricians’ offices has led to a growing divide between healthcare professionals who accept unvaccinated patients and those who do not. This tension stems from the need to balance patients’ rights to make their own healthcare decisions with the responsibility to protect public health. As pediatricians navigate this complex issue, they must consider the potential consequences of their choices on both individual patients and the community.
Examining the Tension between Protecting Public Health and Respecting Patients’ Rights
The right to informed consent is a fundamental principle in healthcare. Patients have the right to make decisions about their own medical care, including whether or not to receive vaccinations. However, the decision to vaccinate is not solely a personal choice, as it has significant implications for public health. Vaccinations help prevent the spread of infectious diseases and protect vulnerable individuals, such as those with compromised immune systems.
Designing a Framework for Pediatricians to Balance Competing Interests
To address the tension between patient autonomy and public health concerns, pediatricians can consider the following framework:
By adopting this framework, pediatricians can engage in a nuanced discussion with their patients about the importance of vaccination while also respecting their autonomy and rights.
Reaching Compromises between Patient Autonomy and Public Health Concerns
In some cases, pediatricians and patients may need to reach compromises that balance individual patient needs with public health concerns. For example:
By working together, pediatricians and patients can find solutions that respect individual patient autonomy while also protecting public health.
Fostering Collaboration and Education
Ultimately, the key to finding a balance between patient autonomy and public health concerns lies in fostering collaboration and education among patients, healthcare professionals, and public health officials. By engaging in open and informed discussions about vaccination policies and procedures, pediatricians can help patients understand the importance of vaccination while also respecting their autonomy and rights. This collaboration can also lead to the development of more effective public health strategies that protect vulnerable individuals and communities.
Building Trust and Understanding
Trust is a critical component in the pediatrician-patient relationship, and vaccination policies can impact this dynamic. By educating patients about the risks and benefits of vaccination and involving them in the decision-making process, pediatricians can build trust and foster understanding about the importance of vaccination. This approach can also help address patient concerns and fears, leading to more informed decision-making and better health outcomes.
Supporting Patients with Vaccine-Related Concerns
Some patients may have legitimate concerns about vaccine safety or effectiveness. Pediatricians can address these concerns by providing accurate and reliable information about vaccines, as well as offering alternatives, such as vaccine exemption forms or delayed vaccination schedules. By supporting patients with vaccine-related concerns, pediatricians can help them make informed decisions about their healthcare while still protecting public health.
Emphasizing Public Health Benefits
Vaccination is a collective effort that benefits the entire community. Pediatricians can emphasize this point by highlighting the public health benefits of vaccination, such as preventing outbreaks and protecting vulnerable individuals. By sharing data and statistics on vaccine efficacy and safety, pediatricians can educate patients about the importance of vaccination and the role it plays in protecting public health.
Prioritizing Compassion and Empathy
Pediatricians must prioritize compassion and empathy when dealing with patients who have concerns about vaccination. By listening to their concerns and providing emotional support, pediatricians can help patients feel heard and understood. This approach can also foster trust and improve the quality of care provided.
Collaborating with Public Health Officials
Pediatricians can collaborate with public health officials to develop local vaccination policies and strategies that balance individual patient needs with community protection. By working together, healthcare professionals and public health officials can develop effective public health strategies that prioritize the well-being of the community.
Engaging in Ongoing Education
The landscape of vaccination policies and practices is constantly evolving. Pediatricians must engage in ongoing education to stay up-to-date on the latest research, recommendations, and best practices. By doing so, they can provide their patients with the information and support they need to make informed decisions about their healthcare.
Addressing Misinformation and Myths
Misinformation and myths about vaccination can be a significant obstacle to informed decision-making. Pediatricians can address these concerns by providing accurate and reliable information about vaccines, as well as countering misinformation and myths with credible sources. By doing so, they can empower patients to make informed decisions about their healthcare.
Respecting Patients’ Rights while Protecting Public Health
Ultimately, pediatricians must strike a balance between respecting patients’ rights to make their own healthcare decisions and protecting public health. By engaging patients in open and informed discussions about vaccination policies and procedures, pediatricians can foster a culture of trust, understanding, and respect that prioritizes both individual patient needs and community protection.
The role of online communities in supporting unvaccinated parents
As the debate surrounding vaccination continues to spark intense conversations, online communities have become a vital source of support for unvaccinated parents. In the face of societal pressure and limited access to accepting pediatricians, these platforms offer a sense of belonging and empowerment. By providing a safe space for individuals to share their experiences, ask questions, and seek advice, online communities are helping to bridge the gap between those who vaccinate and those who do not.
Providing a sense of community
Online forums and social media groups dedicated to unvaccinated families offer a unique opportunity for connections and support. Parents who may feel isolated or stigmatized by their choice can now find others who share their views and values. This community-driven approach fosters a sense of belonging, reducing feelings of loneliness and anxiety that often accompany the decision to opt out of vaccination.
For unvaccinated parents, being part of an online community can be incredibly empowering. By sharing their personal experiences and hearing the stories of others, individuals can gain a deeper understanding of the challenges they face and the importance of their choices. This sense of solidarity helps build confidence and reinforces the notion that they are not alone in their decision.
Online communities often serve as a nexus for valuable resources and information. By connecting with others who have already navigated the path of unvaccinated parenting, individuals can gain access to critical information, research, and recommendations. This can include insights on healthcare providers, vaccination alternatives, and educational materials to support informed decision-making.
Experienced parents within these communities often share their expertise and offer guidance on various topics related to unvaccinated parenting. This advice can range from recommendations for pediatricians to tips on navigating school regulations and social interactions. By tapping into the collective knowledge of these communities, individuals can make more informed decisions and better equip themselves for the challenges ahead.
Online communities also play a crucial role in addressing misconceptions and stigma surrounding unvaccinated parenting. By fostering open discussions and sharing accurate information, these platforms help to dispel myths and misconceptions that may contribute to social isolation. This, in turn, promotes greater understanding and acceptance.
Supporting parents in their journeys
Online communities can play a vital role in supporting parents as they navigate the complexities of unvaccinated parenting. By providing a platform for sharing experiences and seeking advice, these communities can help individuals stay informed, connected, and empowered.
Within these communities, parents often share their personal stories of overcoming obstacles and finding accepting pediatricians. These stories serve as a testament to the determination and resilience of unvaccinated families and can inspire others to take action.
Parents in these communities frequently provide valuable resources and recommendations for navigating the challenges of unvaccinated parenting. This can include tips on finding accepting healthcare providers, managing social interactions, and accessing alternative vaccination options.
Experienced parents within these communities often share their expertise and offer guidance on various topics related to unvaccinated parenting. This advice can range from recommendations for pediatricians to insights on navigating school regulations and social interactions.
Some online communities may provide specialized support groups for parents facing unique challenges, such as caring for children with compromised immune systems or managing chronic health conditions. These groups offer a safe space for individuals to connect with others who understand their struggles and share their experiences.
Effective Communication Strategies for Pediatricians Working with Unvaccinated Parents
Effective communication is a crucial aspect of managing relationships between pediatricians and parents, especially when it comes to discussing vaccination decisions. When interacting with parents who have concerns or hesitations about vaccination, pediatricians should use a non-judgmental and empathetic approach to create a safe space for open dialogue. By employing active listening skills and tailoring their communication to each family’s unique needs, pediatricians can build trust and foster a collaborative atmosphere that supports their patients’ well-being.
Key Considerations for Pediatricians
When interacting with unvaccinated parents, pediatricians must be mindful of several key considerations. These include the parents’ level of understanding about vaccination risks and benefits, their personal and cultural values, and any previous negative experiences they may have had with healthcare providers. Pediatricians should approach each family with an open mind, acknowledging the complexity of vaccine-related concerns and the need for tailored education and support.
Communicating with Clarity and Empathy
Effective communication involves using clear, non-judgmental language to educate and support unvaccinated parents. This requires pediatricians to prioritize active listening, avoid being confrontational, and focus on building a relationship based on trust and mutual respect. When engaging with hesitant parents, pediatricians should aim to create a safe space for open conversation, addressing questions and concerns in a straightforward and compassionate manner.
Empowering Parental Autonomy
Pediatricians should strive to empower parents by fostering an environment that supports informed decision-making. By sharing accurate, unbiased information about vaccine risks and benefits, pediatricians can help parents make informed choices about vaccination. It is essential for pediatricians to respect parents’ autonomy while also acknowledging the ethical responsibility to protect public health.
“Parents want to do what’s best for their children, and pediatricians should empower them to make informed decisions about vaccination.”
Building Trust Between Pediatricians and Unvaccinated Families
Establishing trust between healthcare providers and unvaccinated families is crucial in providing quality care and promoting a positive healthcare experience. A trusting relationship can help alleviate fears and concerns, allowing families to feel more comfortable discussing their medical needs and making informed decisions about their child’s healthcare.
Building trust is a two-way process that requires effort and commitment from both sides. Pediatricians must be willing to listen, understand, and respect the values and concerns of unvaccinated families. At the same time, families must be open to receiving accurate information and guidance from their healthcare providers.
The Importance of Active Listening
Active listening is a fundamental component of building trust in any relationship. When communicating with unvaccinated families, pediatricians should strive to listen attentively to their concerns, ask thoughtful questions, and provide clear, concise responses.
By demonstrating an genuine interest in understanding their concerns, pediatricians can help families feel heard and valued, which can lead to a stronger, more trusting relationship.
Key Strategies for Building Trust
While building trust may require time and effort, there are several strategies that pediatricians can use to establish a strong and supportive relationship with unvaccinated families:
These strategies can help pediatricians establish a strong foundation of trust with unvaccinated families, fostering a positive and supportive healthcare experience.
Empathy and Compassion in Healthcare
Providing care that is sensitive to families’ emotional needs is essential for building trust and ensuring a positive healthcare experience. Pediatricians should strive to demonstrate empathy and compassion in their interactions with families, acknowledging the emotional challenges associated with making decisions about vaccination.
By acknowledging the challenges and emotional complexities involved in vaccination decisions, pediatricians can help families feel more at ease, which can lead to a stronger, more trusting relationship.
Challenges and Opportunities
While building trust with unvaccinated families can be challenging, there are also opportunities for growth and connection. Pediatricians can use these opportunities to educate families about the benefits of vaccination and the importance of preventive care.
By working closely with families and advocating for their health needs, pediatricians can help ensure that all children receive the care they need to thrive.
Closure
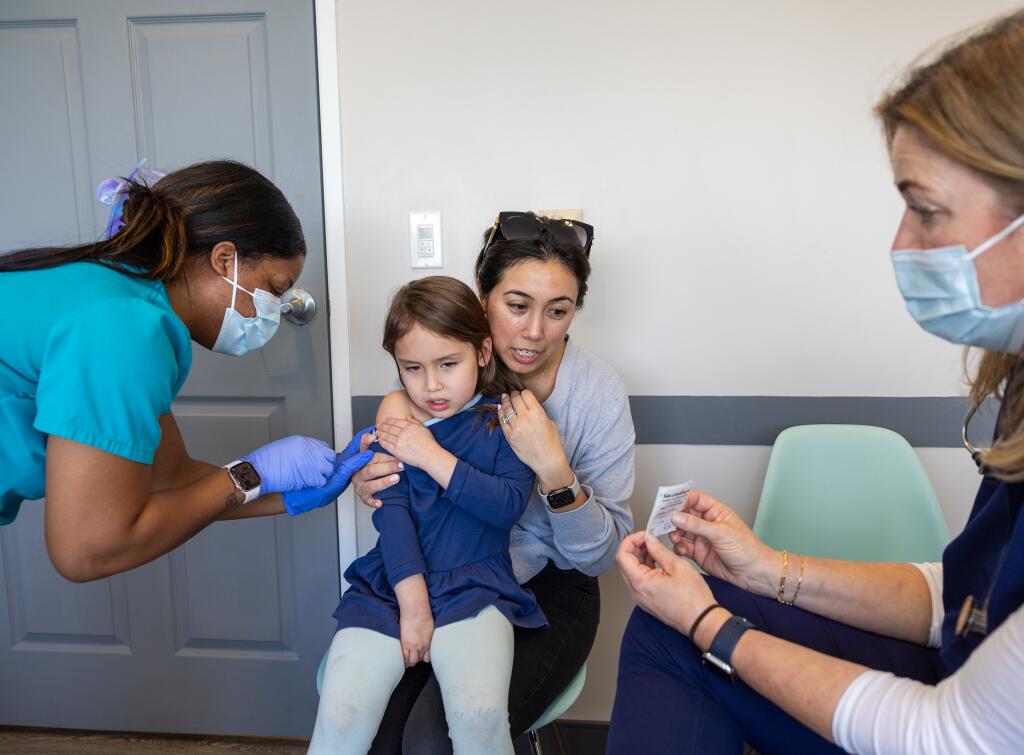
In conclusion, finding pediatricians who accept unvaccinated patients near me requires patience, persistence, and a willingness to explore alternative healthcare options. By understanding the cultural and socioeconomic factors that shape pediatricians’ attitudes towards unvaccinated patients, individuals can begin to build trust and find healthcare that truly puts their loved ones first.
Quick FAQs
How do I find pediatricians who accept unvaccinated patients near me?
You can search online directories, ask for referrals from friends or family members, or contact your local health department for a list of pediatricians who accept unvaccinated patients.
What are the biggest challenges faced by individuals looking for pediatricians who accept unvaccinated patients?
Rural communities, lack of resources, and limited access to healthcare professionals who share their values and beliefs are some of the challenges faced by individuals and families in search of pediatricians who accept unvaccinated patients.
What are the potential consequences of widespread unvaccination among children?
The potential consequences include the spread of infectious diseases, increased risk of serious health complications, and financial burdens on families and the healthcare system.