Glaucoma specialist near me sets the stage for this narrative, offering readers a glimpse into a story that is rich in detail, brimming with originality from the outset.
The process of finding a glaucoma specialist involves understanding the importance of consulting a specialist in diagnosing and treating the condition, as well as learning about the role of a glaucoma specialist in differentiating between various types of glaucoma.
Consulting a Glaucoma Specialist: Early Detection and Effective Treatment
When it comes to diagnosing and treating glaucoma, consulting a glaucoma specialist is of utmost importance. These medical professionals have extensive knowledge and experience in identifying the various types of glaucoma and implementing the most effective treatment plans. Consulting a glaucoma specialist is crucial for early detection, which can significantly impact the quality of life and prognosis for individuals affected by the condition.
Glaucoma specialists can differentiate between various types of glaucoma, including open-angle glaucoma, angle-closure glaucoma, normal-tension glaucoma, and congenital glaucoma. Each type requires a unique approach to treatment, and a glaucoma specialist is equipped to recognize the specific characteristics and symptoms associated with each condition. By working with a glaucoma specialist, individuals can receive a comprehensive diagnosis and personalized treatment plan tailored to their specific needs.
Why Consult a Glaucoma Specialist?
Consulting a glaucoma specialist is essential for several reasons. Firstly, these medical professionals have advanced training and expertise in glaucoma diagnosis and treatment. They use the latest technologies and methodologies to diagnose glaucoma, including visual field testing, tonometry, and optical coherence tomography (OCT). Additionally, glaucoma specialists stay up-to-date with the latest research and treatments, ensuring that patients receive the most effective care available.
- Glaucoma Specialists Have Advanced Training and Expertise: Glaucoma specialists undergo extensive training and education to stay current with the latest advancements in glaucoma diagnosis and treatment. They have a deeper understanding of the complex anatomy and function of the eye, which enables them to identify subtle changes that may indicate glaucoma.
- Latest Technologies and Methodologies: Glaucoma specialists utilize the latest technologies and methodologies, such as advanced imaging tests and surgical procedures, to diagnose and treat glaucoma. These cutting-edge tools enable them to provide more accurate diagnoses and effective treatment plans.
- Personalized Treatment Plans: Glaucoma specialists take a patient-centric approach to treatment, creating personalized plans that address the unique needs and circumstances of each individual. This approach ensures that patients receive the most effective treatment possible.
Scheduling an Appointment and Preparing for a Consultation
To schedule an appointment with a glaucoma specialist, individuals can start by consulting with their primary care physician or optometrist. They can also search online for glaucoma specialists in their area or contact their local eye care association for referrals. Once an appointment is scheduled, individuals can prepare for their consultation by:
- Gathering Medical History: Individuals should gather their medical history, including any previous eye conditions or treatments.
- Bringing Questions: It’s essential to write down questions and concerns to discuss during the consultation, ensuring that all aspects of their condition are addressed.
- Providing Accurate Information: Individuals should provide accurate and detailed information about their symptoms, medical history, and any previous treatments.
- Following Instructions: They should follow any instructions provided by the glaucoma specialist or their staff before the appointment, such as undergoing vision tests or providing medical records.
By following these steps and consulting a glaucoma specialist, individuals can receive the expert care and treatment they need to manage their glaucoma effectively.
Screening Tests and Diagnostic Procedures
Glaucoma diagnosis relies heavily on timely and accurate screening tests and diagnostic procedures. These tests help identify the presence and progression of glaucoma, enabling glaucoma specialists to implement effective treatment plans. The purpose of these screenings is to evaluate the eyes’ internal and external structures for potential damage caused by glaucoma.
Visual Field Testing
Visual field testing is an essential diagnostic procedure in glaucoma diagnosis. It evaluates the field of vision by detecting any blind spots or losses of peripheral vision. Visual field tests measure the eyes’ ability to detect light and colors, helping glaucoma specialists detect potential damage to the optic nerve.
Examples of visual field tests include the Humphrey Visual Field Test, the Goldmann kinetic perimetry, and the Octopus perimetry.
During the test, patients are typically seated in a dark room and asked to focus on a central point while responding to a series of flashing lights. These lights vary in intensity, color, and location, helping the doctor detect any vision loss.
Pressure Measurements
Pressure measurements are a crucial component of glaucoma diagnosis. Glaucoma specialists use various methods to measure eye pressure, which is essential in determining the presence and severity of glaucoma. High eye pressure is a significant risk factor for glaucoma, as it can damage the optic nerve.
- Goldmann Applanation Tonometry: This method uses a thin strip of metal to flatten a small portion of the cornea, measuring the pressure inside the eye.
- Rebound Tonometry: This method uses a small probe to rapidly touch the cornea, measuring the pressure inside the eye.
- Non-contact tonometry: This method uses a puff of air to measure the pressure inside the eye.
Imaging Tests
Imaging tests play a vital role in glaucoma diagnosis and management. Glaucoma specialists use various imaging tests, including Optical Coherence Tomography (OCT) and fundus photography, to evaluate the optic nerve and retinal ganglion cell layer.
- Optical Coherence Tomography (OCT): This non-invasive imaging test provides detailed cross-sectional images of the retina and optic nerve, helping glaucoma specialists detect potential damage.
- Fundus Photography: This imaging test captures a color photograph of the retina, displaying the blood vessels and optic nerve area.
- Scanning Laser Polarimetry (SLP): This imaging test uses a laser to create a detailed image of the retinal nerve fiber layer.
Imaging tests can be performed on their own or in conjunction with other diagnostic procedures, providing glaucoma specialists with a comprehensive understanding of the condition.
Fundus Examination
Fundus examination is an essential part of glaucoma diagnosis. Glaucoma specialists use an ophthalmoscope to examine the retina and optic nerve, searching for signs of glaucoma, such as cupping, vessels, and retinal hemorrhages. A fundus examination can detect the early signs of glaucoma, aiding in early intervention.
- Cupping: This condition refers to the thinning and excavation of the optic disc, creating a cup-like appearance.
- Retinal Hemorrhages: These blood-filled vessels occur due to damage from the increased eye pressure.
- Optic Nerve Damage: The presence of optic nerve damage is often associated with increased eye pressure and can be detected through a fundus examination.
Fundus examination is crucial for detecting the early signs of glaucoma and guiding treatment options.
Electrophysiology Tests
Electrophysiology tests assess the electrical activity of the retina and optic nerve. Glaucoma specialists use these tests to evaluate the function of the retina and optic nerve, providing valuable information about the severity of glaucoma.
- Visual Evoked Potentials (VEP) Test: This test measures the electrical activity of the visual cortex, helping glaucoma specialists assess the integrity of the optic nerve.
- Electroretinography (ERG) Test: This test measures the electrical activity of the retina, aiding in the detection of retinal damage.
Electrophysiology tests play a crucial role in understanding the effects of glaucoma on the retina and optic nerve, guiding treatment options, and evaluating disease progression.
Ultrasound Tests
Ultrasound tests use sound waves to create images of the eye and its surrounding structures. Glaucoma specialists use these tests to assess the optic nerve, detect potential damage, and evaluate the severity of glaucoma.
- Sonography: This test uses sound waves to create images of the optic nerve and surrounding tissues.
- Biometry: This test measures the length and curvature of the eyeball, helping glaucoma specialists determine the correct intraocular lens power.
Ultrasound tests are essential in evaluating the optic nerve and surrounding structures, aiding in early detection and monitoring of glaucoma progression.
Treatment Options and Management Strategies
Glaucoma is a chronic condition that requires ongoing management and treatment to slow down vision loss and prevent further damage. A glaucoma specialist will work with you to develop a personalized treatment plan that takes into account your unique needs and medical history.
Medications for Glaucoma Treatment
Medications are often the first line of treatment for glaucoma, and they come in various forms, including eye drops, oral medications, and injectables. The goal of medication is to reduce eye pressure and slow down vision loss. There are several types of medications available, each with its own mechanism of action:
* Beta blockers: These medications, such as timolol and levobunolol, slow down the production of aqueous humor, which is the fluid in the eye that contributes to eye pressure.
* Alpha agonists: These medications, such as brimonidine and apraclonidine, reduce the outflow of aqueous humor, which also helps to lower eye pressure.
* Prostaglandin analogs: These medications, such as latanoprost and bimatoprost, increase the outflow of aqueous humor, which helps to lower eye pressure.
* Carbonic anhydrase inhibitors: These medications, such as acetazolamide and dorzolamide, reduce the production of aqueous humor.
Surgical Treatment Options for Glaucoma
Surgery may be necessary if medications and other treatments are not effective in controlling eye pressure and preventing vision loss. There are several types of surgical procedures for glaucoma, including:
* Trabeculectomy: This surgery involves creating a new drainage channel in the eye to allow excess fluid to drain out. This helps to lower eye pressure and prevent vision loss.
* Trabeculoplasty: This surgery involves using a laser to create holes in the trabecular meshwork, which is the tissue that drains excess fluid from the eye.
* Glaucoma drainage devices: These devices, such as the Ahmed valve and the Baerveldt glaucoma implant, are surgically implanted in the eye to help drain excess fluid and lower eye pressure.
* Minimally invasive glaucoma surgery (MIGS): This type of surgery involves using small incisions and advanced technology to create new drainage channels in the eye.
Regular Eye Exams and Follow-Up Appointments
Regular eye exams and follow-up appointments are crucial in managing glaucoma. These appointments allow your glaucoma specialist to monitor your condition, adjust your treatment plan as needed, and perform diagnostic tests to assess the effectiveness of your treatment.
Personalized Treatment Plans, Glaucoma specialist near me
Developing a personalized treatment plan with your glaucoma specialist involves working together to identify the best course of treatment for your unique needs and medical history. This may involve:
* Creating a treatment plan that incorporates multiple medications and/or surgical procedures
* Conducting regular follow-up appointments to monitor your condition and adjust your treatment plan as needed
* Performing regular eye exams to assess the effectiveness of your treatment
* Educating you on the importance of adherence to your treatment plan and the risks of non-compliance
* Collaborating with other healthcare professionals, such as optometrists and primary care physicians, to ensure comprehensive care for your glaucoma.
Advances in Glaucoma Detection and Treatment
The field of glaucoma care has witnessed significant advancements in recent years, driven by innovation in technology, research, and collaboration between healthcare professionals. These developments have improved diagnosis, treatment, and patient outcomes.
The introduction of artificial intelligence (AI) in glaucoma detection has revolutionized the field. AI-powered algorithms can analyze retinal images and detect signs of glaucoma with high accuracy, allowing for early intervention and potentially preventing vision loss. Portable diagnostic devices, such as tonometers and pachymeters, have also become more accessible and user-friendly, facilitating screening and monitoring in diverse settings.
Advancements in Imaging Technologies
Advances in imaging technologies have significantly improved glaucoma diagnosis and monitoring. Optical coherence tomography (OCT) and swept-source OCT (SS-OCT) have enhanced the detection of retinal nerve fiber layer thinning, optic disc changes, and other indicators of glaucoma. These high-resolution imaging modalities enable more precise assessment of disease progression and treatment response, ultimately benefiting patients.
Emergence of Portable Diagnostic Devices
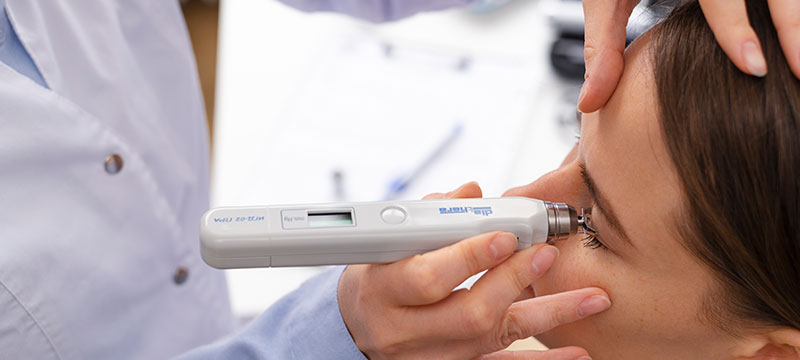
Portable diagnostic devices have streamlined glaucoma screening and monitoring, particularly in community-based settings and developing regions. These devices, often featuring advanced sensors and algorithms, can accurately measure intraocular pressure (IOP), corneal thickness, and other critical parameters.
Key Benefits of Portable Diagnostic Devices:
* Rapid and accurate IOP measurements
* Enhanced convenience for patients and healthcare providers
* Easy transportation and storage, facilitating outreach services
* Improved access to glaucoma detection and monitoring in underserved communities
Future Directions in Glaucoma Research
Ongoing research and innovation aim to further improve glaucoma detection, treatment, and patient outcomes. Emerging areas of focus include:
* Development of new glaucoma biomarkers and imaging modalities
* Advanced materials and devices for glaucoma treatment, such as injectable medications and implantable pumps
* Integration of AI and machine learning to enhance glaucoma diagnosis and treatment planning
* Collaborative efforts to reduce healthcare disparities and improve access to care
Impact of Emerging Technologies
The introduction of emerging technologies in glaucoma care has significant implications for patients and healthcare providers. By leveraging AI, portable diagnostic devices, and other innovations, clinicians can:
* Improve early detection and intervention rates
* Enhance treatment efficacy and safety
* Personalize patient care based on advanced imaging and biomarker analysis
* Expand access to high-quality glaucoma care for underserved populations
Coping with Glaucoma and Maintaining Eye Health: Glaucoma Specialist Near Me

Managing glaucoma effectively requires a multifaceted approach that incorporates healthy lifestyle habits, regular monitoring with your glaucoma specialist, and adherence to your prescribed treatment plan. By adopting a proactive approach to maintaining your eye health, you can reduce the risk of vision loss and manage your condition with confidence.
A healthy lifestyle is the foundation of effective glaucoma management. Engaging in regular physical activity, such as brisk walking, cycling, or swimming, can lower your blood pressure and improve circulation to your eyes. Additionally, a balanced diet rich in fruits, vegetables, and whole grains provides essential nutrients for maintaining optimal eye health.
Staying Connected with Your Glaucoma Specialist
Regular follow-up appointments with your glaucoma specialist are crucial for monitoring your condition and adjusting your treatment plan as needed. Your specialist will assess your vision, ocular pressure, and other factors to determine the effectiveness of your current treatment. Collaborate with your specialist to:
- Discuss any changes in your vision or symptoms, such as blurred vision, eye pain, or redness.
- Share any concerns or questions you may have about your treatment plan.
- Review your treatment goals and adjust your plan accordingly.
- Discuss any lifestyle changes or modifications you can make to support your eye health.
- Undergo regular ocular imaging tests, such as optic nerve scans or retinal scans, to monitor your condition.
It is essential to be open and honest with your glaucoma specialist about your treatment concerns and progress. Your specialist is committed to helping you manage your glaucoma effectively and prevent vision loss.
Healthy Lifestyle Habits for Managing Glaucoma
A healthy lifestyle plays a vital role in managing glaucoma. Adopting the following habits can help you maintain optimal eye health:
- Get regular exercise: Engage in at least 30 minutes of moderate-intensity physical activity per day to lower your blood pressure and improve circulation to your eyes.
- Maintain a balanced diet: Eat a diet rich in fruits, vegetables, and whole grains to provide essential nutrients for maintaining optimal eye health.
- Manage stress: High stress levels can exacerbate glaucoma symptoms. Engage in stress-reducing activities, such as meditation or yoga, to help manage stress.
- Don’t smoke: Smoking can increase your risk of developing glaucoma and worsen existing symptoms. Quit smoking to protect your eye health.
By incorporating these healthy lifestyle habits into your daily routine, you can take proactive steps towards managing your glaucoma and maintaining good eye health.
Monitoring Your Treatment Progress
Regular monitoring with your glaucoma specialist is crucial for tracking your treatment progress and making any necessary adjustments. Your specialist will assess your vision, ocular pressure, and other factors to determine the effectiveness of your current treatment. Collaborate with your specialist to:
- Undergo regular ocular imaging tests, such as optic nerve scans or retinal scans, to monitor your condition.
- Discuss any changes in your vision or symptoms with your specialist.
- Review your treatment goals and adjust your plan accordingly.
By working closely with your glaucoma specialist and adopting healthy lifestyle habits, you can effectively manage your glaucoma and maintain good eye health.
Glaucoma is a progressive condition that requires ongoing management and attention. By staying connected with your glaucoma specialist and adopting healthy lifestyle habits, you can reduce the risk of vision loss and manage your condition with confidence.
Common Myths and Misconceptions about Glaucoma
Glaucoma is a complex eye condition that affects millions of people worldwide. Unfortunately, many myths and misconceptions surround glaucoma, which can lead to misinformed decisions and inadequate treatment. It is essential to debunk these myths and provide accurate information to help patients make informed decisions about their glaucoma treatment.
Myth: Glaucoma only affects older people
While it is true that glaucoma is more common among older adults, it can affect anyone, regardless of age. In fact, glaucoma can affect people of all ages, including infants and young children. According to the National Eye Institute, glaucoma is a leading cause of vision loss in people under the age of 40. This is why regular eye exams are crucial, especially for those with a family history of glaucoma.
Myth: Glaucoma is a painless condition
Glaucoma can be a painless condition, but it can also cause significant discomfort, including eye pressure, headaches, and blurred vision. In some cases, patients may experience eye pain, redness, and sensitivity to light. These symptoms can be a sign of an underlying condition, such as acute angle-closure glaucoma, which requires immediate medical attention.
Myth: Glaucoma can be cured
Unfortunately, glaucoma is a chronic condition that cannot be cured. However, with proper treatment and management, it is possible to slow or stop the progression of the disease. Treatment options, such as eye drops, oral medications, or surgery, can help control eye pressure and prevent further vision loss.
Myth: Glaucoma only affects the eyes
Glaucoma can have a significant impact on a person’s quality of life, beyond just their vision. Untreated glaucoma can lead to blindness, which can affect a person’s independence, mobility, and overall well-being. Additionally, glaucoma can also increase the risk of other health conditions, such as heart disease, stroke, and diabetes.
Myth: Glaucoma is a rare condition
Glaucoma is a relatively common condition, affecting over 3 million people in the United States alone. According to the National Eye Institute, glaucoma is a leading cause of vision loss among Americans, accounting for 9% to 12% of all cases of blindness. This highlights the importance of regular eye exams and awareness about glaucoma.
Myth: You can only develop glaucoma if you have a family history
While having a family history of glaucoma increases the risk, it is not the only factor. Other risk factors, such as age, genetics, and medical conditions, can also contribute to the development of glaucoma. Factors such as high eye pressure, thin corneas, and certain medical conditions, such as diabetes or high blood pressure, can also increase the risk.
Myth: Glaucoma treatment is expensive
While some glaucoma treatments can be expensive, many are covered by insurance and can be managed on a budget. Additionally, early detection and treatment can help prevent costly complications, such as blindness and hospitalization.
Myth: Glaucoma cannot be treated with eye drops
Eye drops are a common and effective treatment for glaucoma. In fact, eye drops are often the first line of treatment, as they can help reduce eye pressure and prevent further vision loss. However, in some cases, oral medications or surgery may be necessary to control eye pressure.
Myth: Glaucoma is a solitary disease
Glaucoma is often associated with other health conditions, such as cataracts, macular degeneration, and diabetic retinopathy. In fact, a study by the National Eye Institute found that people with glaucoma are at higher risk of developing other eye diseases. This highlights the importance of regular eye exams to detect and manage multiple eye conditions.
Myth: Glaucoma only affects the vision of one eye
Glaucoma can affect both eyes, although it often begins in one eye before affecting the other. If left untreated, glaucoma can lead to vision loss in both eyes, making it essential to seek medical attention as soon as possible.
Myth: Glaucoma is not preventable
While glaucoma cannot be prevented, regular eye exams can help detect the condition early, allowing for timely treatment and preventing further vision loss. By adopting a healthy lifestyle, including regular exercise, a balanced diet, and not smoking, you can reduce your risk of developing glaucoma and other eye conditions.
Closing Notes
The content provided a thorough overview of finding a glaucoma specialist near me, highlighting the importance of consulting a glaucoma specialist and understanding the different types of glaucoma.
We hope that this information has been helpful in navigating the complexities of glaucoma care.
Common Queries
What is the importance of consulting a glaucoma specialist?
Consulting a glaucoma specialist is crucial in diagnosing and treating glaucoma, as they have the necessary expertise and training to differentiate between various types of glaucoma.
How do I prepare for a consultation with a glaucoma specialist?
To prepare for a consultation with a glaucoma specialist, it is essential to gather information about your medical history, including any previous eye problems or conditions, and to ask questions during the appointment to ensure that you understand your diagnosis and treatment plan.
What are the different types of glaucoma?
There are several types of glaucoma, including open-angle glaucoma, closed-angle glaucoma, normal-tension glaucoma, and congenital glaucoma, each requiring different treatment approaches and management strategies.
How often should I have eye exams to monitor my glaucoma?
The frequency of eye exams for monitoring glaucoma depends on the severity of the condition and the effectiveness of the treatment plan, but regular follow-up appointments with a glaucoma specialist are crucial in managing the condition.