As doctors who specialize in peripheral neuropathy near me takes center stage, this opening passage beckons readers into a world where advanced treatments and innovative care meet the urgent needs of those living with nerve health issues.
The following sections dive deeper into finding specialists, managing symptoms, preventing and treating the condition, and understanding the causes and types of peripheral neuropathy.
How Can Individuals Find Reputable Doctors Who Specialize in Peripheral Neuropathy near their Location
Peripheral neuropathy, a complex health condition affecting the nerves, requires specialized care from healthcare professionals who possess extensive knowledge and experience in managing the condition. Finding a reputable specialist near your location can significantly impact the effectiveness of treatment and overall well-being.
When seeking a specialist, it’s essential to consider several factors, including the doctor’s experience, expertise, and qualifications in addressing peripheral neuropathy. Here are some steps to help you find a qualified specialist near your location.
Online Directories and Professional Associations
Online directories and professional associations provide a convenient and efficient way to search for doctors who specialize in peripheral neuropathy. Some notable online directories include:
- American Academy of Neurology (AAN) Doctor Finder: A comprehensive database of neurologists who have demonstrated expertise in various neurologic subspecialties, including peripheral neuropathy. You can filter search results by location, medical specialty, and language.
- American Medical Association (AMA) DoctorFinder: A database of licensed physicians, including those specializing in neurological disorders. You can search by name, location, or medical specialty.
- Patient Advocates for Chronic Fatigue Syndrome and Fibromyalgia (PACF) Doctor Directory: A directory of healthcare professionals who have experience in managing chronic diseases, including peripheral neuropathy.
- The Neuropathy Association: Provides a directory of healthcare professionals specializing in neuropathic disorders, along with educational resources and support networks.
These directories often verify a doctor’s credentials and experience, providing added assurance that you’re seeking care from a qualified professional.
Personal Referrals and Word of Mouth
Personal referrals from trusted individuals, such as family members, friends, or primary care physicians, can be invaluable in finding a reputable specialist. Ask for recommendations and discuss your specific needs and concerns with the referral source.
Verifying a Doctor’s Credentials and Experience
Before scheduling an appointment, it’s crucial to verify a doctor’s qualifications and experience in managing peripheral neuropathy. You can do this by:
- Checking the doctor’s professional certifications and licenses on the state’s medical board website.
- Reviewing their educational background and training in the field of neurology.
- Assessing their experience in treating patients with peripheral neuropathy.
- Reading patient reviews and ratings on websites like Healthgrades, RateMDs, or Zocdoc.
By following these steps and taking the time to research and verify a doctor’s credentials, you can increase your chances of finding a reputable specialist near your location who will provide effective care for your peripheral neuropathy condition.
What is the Role of Lifestyle Changes in Preventing and Managing Peripheral Neuropathy
Peripheral neuropathy is a complex condition that can be influenced by various factors, including our lifestyle choices. By adopting healthy habits, individuals can significantly reduce their risk of developing peripheral neuropathy and manage its symptoms. A well-balanced diet, regular exercise, and adequate sleep are essential components of a lifestyle that supports nerve health.
The Impact of Diet on Peripheral Neuropathy
A healthy diet plays a critical role in preventing and managing peripheral neuropathy. Foods rich in antioxidants, such as fruits, vegetables, and whole grains, help protect nerves from damage caused by free radicals. Omega-3 fatty acids found in fatty fish, nuts, and seeds also promote nerve health by reducing inflammation.
- Leafy greens like spinach and kale are excellent sources of antioxidants and folate, which help maintain healthy nerve cells.
- Fish rich in omega-3 fatty acids, such as salmon and tuna, support nerve function and reduce inflammation.
- Complex carbohydrates like whole grains and sweet potatoes provide energy for nerve function.
- Herbs and spices like turmeric and ginger have anti-inflammatory properties that help reduce nerve pain.
The Importance of Exercise in Peripheral Neuropathy Management
Regular exercise is essential for maintaining nerve health and reducing the symptoms of peripheral neuropathy. Exercise promotes blood flow, reducing inflammation and improving nerve function. Aerobic exercises like walking, cycling, and swimming are beneficial for overall health and can help manage peripheral neuropathy symptoms.
- Aerobic exercises like brisk walking, cycling, and swimming improve blood flow and reduce inflammation.
- Resistance exercises like weightlifting and bodyweight exercises help build strength and improve nerve function.
- Mind-body exercises like yoga and tai chi promote relaxation, reducing stress and anxiety that can exacerbate peripheral neuropathy symptoms.
- Regular physical activity also improves sleep quality, which is essential for nerve health.
The Role of Sleep in Peripheral Neuropathy Prevention and Management
Adequate sleep is crucial for maintaining nerve health and preventing peripheral neuropathy. During sleep, the body repairs and regenerates nerve cells, reducing inflammation and improving nerve function. Aim for 7-8 hours of sleep each night to help manage peripheral neuropathy symptoms.
- Establish a bedtime routine to signal the body that it’s time to sleep.
- Create a sleep-conducive environment by keeping the bedroom cool, dark, and quiet.
- Avoid caffeine, nicotine, and electronics before bedtime to promote relaxation.
- Consider keeping a sleep diary to track sleep patterns and identify areas for improvement.
Peripheral neuropathy management requires a comprehensive approach that includes lifestyle changes, medical treatment, and self-care strategies. By adopting healthy habits, individuals can reduce their risk of developing peripheral neuropathy and improve their overall quality of life.
Warning Signs and Risk Factors Associated with Peripheral Neuropathy

Peripheral neuropathy, a condition characterized by nerve damage, can manifest in various ways, requiring prompt medical attention when symptoms worsen or exhibit rapid progression. Understanding the warning signs and associated risk factors can aid in timely diagnosis and intervention.
Rapid Nerve Damage Progression Indicators
A sudden increase in severity of symptoms necessitates immediate medical attention. These include:
- Rapid expansion or intensification of pain, numbness, or weakness in the affected areas.
- Increased sensitivity to touch or vibrations in the extremities, which may signal the spread of damage to more nerves.
- Abnormal sensations such as burning, tingling, or a pins-and-needles feeling, which may worsen with physical activity or rest.
- Difficulty controlling movements or maintaining balance due to progressive weakness.
Common Underlying Conditions
Certain conditions and health issues are commonly linked to peripheral neuropathy, making early detection and management crucial in preventing further complications. Some of these risk factors include:
- Diabetes and Blood Glucose Imbalances – Uncontrolled diabetes is a leading cause of peripheral neuropathy, as high blood sugar levels damage nerve cells.
- Autoimmune Disorders – Conditions such as rheumatoid arthritis and lupus may cause inflammation and damage to the nerves.
- Infections and Infectious Diseases – Bacterial, viral, and fungal infections can damage nerves, particularly if left untreated or with delayed treatment.
- Medication Side Effects and Toxicity – Certain pharmaceuticals, such as chemotherapy agents and certain antibiotics, can lead to peripheral neuropathy.
- Thiamine Deficiency (Vitamin B1) – People with chronic alcohol use, malnutrition, or eating disorders are vulnerable to thiamine deficiency and its neurological consequences.
- Heredity and Genetics – Families with a history of specific types of neuropathy may be at a higher risk of developing related conditions.
- Smoking and Substance Abuse – Long-term use of tobacco, cocaine, or other stimulants increases the risk of nerve damage due to oxidative stress and inflammation.
- Physical Trauma and Injury – Fractures, amputations, or severe bruises can potentially cause nerve damage.
Age-Related Factors, Doctors who specialize in peripheral neuropathy near me
Nerve damage is often age-related, with many cases arising in middle-aged individuals or later. Understanding how age plays a role helps patients be more aware of symptoms related to their age, which can aid in identifying early warning signs and risk factors.
According to the National Institute of Neurological Disorders and Stroke (NINDS), approximately 60% of individuals experience some form of peripheral neuropathy by the age of 60.
Types and Causes of Peripheral Neuropathy and Their Impact on Patient Outcomes
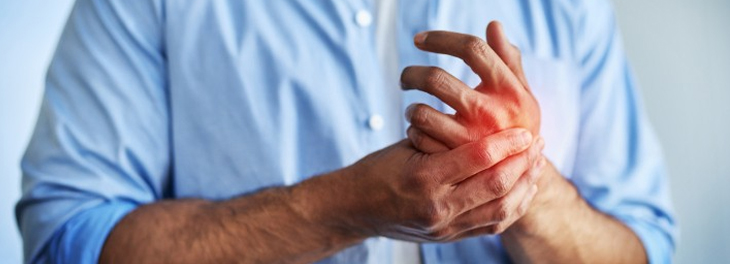
Peripheral neuropathy encompasses a range of conditions that affect the nerves outside the brain and spinal cord, leading to various symptoms and degrees of impairment. Understanding the different types and causes of peripheral neuropathy is essential for developing effective treatment plans and improving patient outcomes. This discussion will explore the distinct characteristics of several common types of peripheral neuropathy, including diabetic neuropathy, chemotherapy-induced neuropathy, and hereditary neuropathy.
Diabetic Neuropathy: A Leading Cause of Peripheral Neuropathy
Diabetic neuropathy is a result of high blood sugar levels damaging nerve fibers over time, leading to a range of symptoms including numbness, tingling, and pain in the hands and feet. It is a common complication of diabetes and can significantly impact a patient’s quality of life. Factors such as duration of diabetes, blood sugar control, and presence of other health conditions contribute to the development and progression of diabetic neuropathy. Understanding these factors is crucial for developing a personalized treatment plan that addresses the underlying causes of the condition.
- Numbness and tingling sensations in hands and feet
- Pain and burning sensations in extremities
- Weakness and loss of motor function
- Blistering and open sores on the feet, leading to increased risk of infection
Chemotherapy-Induced Neuropathy: A Common Side Effect of Cancer Treatment
Chemotherapy-induced neuropathy is a prevalent side effect of cancer treatment, affecting up to 40% of chemotherapy patients. This type of peripheral neuropathy is caused by damage to nerve fibers as a result of cancer medication. Symptoms include numbness, tingling, and pain in the hands and feet, as well as sensitivity to temperature changes. The severity and duration of chemotherapy-induced neuropathy vary depending on the type and dosage of chemotherapy, as well as individual patient factors such as age and overall health.
- Numbness and tingling sensations in hands and feet
- Pain and burning sensations in extremities
- Sensitivity to temperature changes
- Weakness and loss of motor function
Hereditary Neuropathy: A Genetic Condition Affecting Nerve Function
Hereditary neuropathy, also known as Charcot-Marie-Tooth disease, is a group of genetic disorders that affect the nerves and their function. This condition is inherited from one’s parents and can manifest at any age, depending on the genetic mutation. Symptoms include weakness and loss of motor function in the hands and feet, as well as numbness and tingling sensations. Hereditary neuropathy can significantly impact a patient’s quality of life, requiring ongoing management and treatment to slow disease progression.
According to the National Institute of Neurological Disorders and Stroke (NINDS), hereditary neuropathy affects approximately 1 in 2,500 individuals worldwide.
Implications for Treatment Choice and Patient Prognosis
Understanding the different types and causes of peripheral neuropathy is essential for developing effective treatment plans and improving patient outcomes. Each type of peripheral neuropathy requires a personalized approach, taking into account the underlying causes, symptoms, and individual patient factors. Treatment options for peripheral neuropathy include medication, physical therapy, and lifestyle modifications, such as dietary changes and exercise programs.
Final Wrap-Up: Doctors Who Specialize In Peripheral Neuropathy Near Me
In conclusion, finding the right specialist for peripheral neuropathy care is an essential step towards achieving optimal treatment outcomes and managing symptoms effectively. By understanding the condition, its causes, and the different types, patients can work closely with their healthcare team to develop a personalized treatment plan and improve their quality of life.
Questions Often Asked
Q: What are the primary symptoms of peripheral neuropathy?
A: Common symptoms include numbness, pain, tingling sensation, weakness, and loss of reflexes in the hands and feet.
Q: What is the best way to find a specialist near me?
A: You can search online directories such as Google, professional associations like the American Academy of Neurology, and ask for personal referrals from friends and family.
Q: Can lifestyle changes help prevent or manage peripheral neuropathy?
A: Yes, adopting healthy habits such as a balanced diet, regular exercise, and adequate sleep can help manage symptoms and prevent progression of the condition.
Q: What are some common underlying conditions that contribute to peripheral neuropathy?
A: Diabetes, chemotherapy, viral infections, and autoimmune disorders are some of the underlying conditions that can lead to peripheral neuropathy.
Q: What is the role of a healthcare team in managing peripheral neuropathy?
A: A healthcare team plays a crucial role in developing a comprehensive treatment plan, monitoring symptoms, and adjusting treatment as needed to achieve optimal outcomes.