Bone grafts near me are a surgical procedure that involves transplanting bone tissue from one part of the body to another to repair or replace damaged or missing bone. This innovative treatment option has revolutionized the field of orthopedic and dental surgery, allowing patients to regain their confidence and mobility. Whether you’re dealing with a sports injury, a congenital defect, or the aftermath of a traumatic accident, bone grafts are a viable solution that can significantly improve your quality of life.
In this comprehensive guide, we’ll delve into the world of bone grafts near me, exploring the different types of bone grafts, preparation for surgery, the bone grafting procedure, recovery and postoperative care, and the factors influencing success rates and outcomes. We’ll also discuss alternative treatments and emerging technologies in the field of regenerative medicine.
Understanding the Purpose and Indications for Bone Grafts
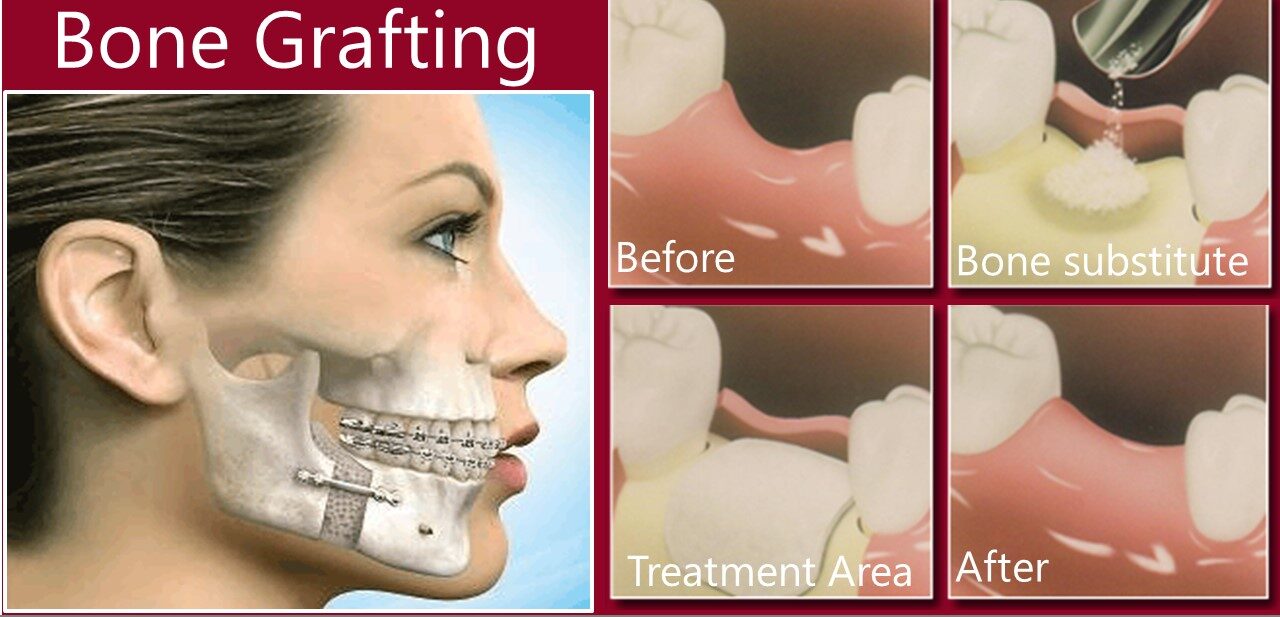
Bone grafts, also known as bone transplantation, involve transferring bone tissue from one part of the body to another to repair or regenerate damaged bone. This surgical intervention has been extensively utilized in orthopedic, maxillofacial, and oral surgeries to address various medical conditions. Bone grafts are a crucial treatment option for individuals with bone defects, fractures, or degenerative disorders that require bone reconstruction to maintain or restore form, function, and quality of life.
Benefits of Bone Grafts
Bone grafts have revolutionized the field of medicine by offering numerous advantages over alternative treatments. Some of the key benefits include:
- Autologous Bone Grafts
- Allogenic Bone Grafts
- Xenogenic Bone Grafts
- Synthetic Bone Grafts
- A comprehensive medical history and physical examination to identify any underlying medical conditions that may affect the surgery
- Blood work, including complete blood counts, blood chemistry tests, and coagulation studies, to assess the patient’s overall health and identify any potential bleeding disorders or other medical conditions
- Infectious disease testing, such as blood tests for HIV and hepatitis, to ensure the patient does not have any infectious diseases that could compromise the surgery
- X-rays or other imaging studies, such as computed tomography (CT) or magnetic resonance imaging (MRI), to evaluate the extent and severity of the bone defect or deformity
- A dental evaluation to assess the patient’s oral health and identify any potential risks associated with bone graft surgery
- Open Approach: This traditional approach involves making a large incision in the skin to access the bone tissue. It allows for greater visibility and manipulation of the bone, making it ideal for complex bone reconstructions.
- Minimally Invasive Approach: This approach uses smaller incisions and specialized instruments to minimize tissue damage and scarring. It is ideal for smaller bone defects and procedures that require less extensive bone manipulation.
- Drills and Burrs: These instruments are used to create holes and shape the bone tissue, allowing for precise placement of the graft.
- Files and Rasp: These instruments are used to smooth and shape the bone surface, ensuring a seamless integration of the graft.
- Forceps and Pickups: These instruments are used to gently grasp and manipulate the bone tissue, allowing for precise placement and fixation of the graft.
-
Step 1: Harvesting the Bone Graft
-
Step 2: Preparing the Recipient Site
-
Step 3: Placing the Bone Graft
-
Step 4: Securing the Bone Graft
- Younger patients (under 40 years old) generally have better bone quality and a faster healing process.
- Patient older than 60 may experience decreased bone density and a slower healing process.
-
Smokers are more likely to experience delayed bone healing and a higher risk of complications.
- Patients who quit smoking at least 3 months before surgery tend to have better outcomes.
- A balanced diet rich in calcium and vitamin D is essential for optimal bone health.
- Patients with malnutrition or a history of eating disorders may require additional attention and support.
Faster and More Reliable Healing
Bone grafts facilitate faster and more reliable healing by providing a viable source of living tissue. This reduces the likelihood of complications and promotes better bone integration.
Improved Bone Density
By incorporating donor bone tissue, bone grafts increase bone density and enhance the structural integrity of the affected area.
Enhanced Bone Growth and Regeneration
Bone grafts stimulate bone growth and regeneration by introducing a scaffold for mesenchymal stem cells to migrate and differentiate into bone-forming cells.
Restoration of Lost Functionality
By repairing damaged or deformed bones, bone grafts restore lost functionality and allow patients to regain their mobility and independence.
Increased Treatment Options
Bone grafts expand the range of treatment options available to patients with complex bone defects or fractures, offering a more definitive solution to restore bone integrity and function.
Medical Conditions Requiring Bone Grafts
Bone grafts are commonly employed to address a variety of medical conditions, including:
Orthopedic Conditions
Osteoporosis, non-union fractures, joint degeneration, and developmental bone disorders are among the common orthopedic conditions treated with bone grafts.
Maxillofacial and Oral Surgeries
Bone grafts are utilized in surgical procedures such as dental implant placement, jaw reconstruction, and craniofacial reconstruction following trauma or congenital disorders.
Spine and Neurosurgery
Bone grafts are employed in spine fusion surgeries to repair vertebrae fractures, degenerative disc disease, or scoliosis, as well as to address complex spinal deformities.
Importance of Bone Density and Its Impact on Surgical Outcomes
Bone density is critical to surgical outcomes in bone grafting procedures. Adequate bone density ensures the integration and stability of the graft, allowing for proper healing and restoration of bone function.
| Adequate Bone Density | Poor Bone Density | |
|---|---|---|
| Surgical Outcomes | Faster healing and better integration | Delayed healing and increased risk of complications |
| Long-term Stability | Stable and durable bone reconstruction | Instability and potential for graft failure |
| Regulatory Factors | Effective regulation of calcium and vitamin D levels | Impaired regulation of bone remodeling factors |
Bone density directly influences the success of bone grafting procedures, highlighting the importance of maintaining optimal bone health through a balanced diet, regular exercise, and proper medical management.
Types of Bone Grafts and Materials Used
When considering bone grafts, it’s essential to understand the different types of materials and bone grafts used in medical procedures. These materials vary in their origins, composition, and properties, which determine their suitability for specific applications.
Types of Bone Grafts
There are four primary types of bone grafts: autologous, allogenic, xenogenic, and synthetic. Each type has its unique characteristics, advantages, and applications.
| Types of Bone Grafts | Composition | Properties | Applications |
|---|---|---|---|
| Autologous Bone Grafts | Bone tissue from the patient’s own body | Similar immunological and mechanical properties to native bone | Reconstruction of large bone defects, revision hip and knee surgeries |
| Allogenic Bone Grafts | Bone tissue from a donor | May be immunoreactive, potential risk of disease transmission | Augmentation of facial bone defects, spinal fusion surgeries |
| Xenogenic Bone Grafts | Processed animal bone tissue | May be immunoreactive, risk of disease transmission | Dental bone grafting, periodontal surgery |
| Synthetic Bone Grafts | Man-made materials, such as calcium phosphate and titanium | Non-immunogenic, biocompatible, and biodegradable | Fillers for bone defects, spinal fusion surgeries, and orthopedic applications |
Preparation for Bone Graft Surgery
Before undergoing a bone graft surgery, patients must undergo thorough pre-operative assessments and testing to ensure their safety and the success of the procedure. These evaluations typically involve a series of medical tests, imaging studies, and consultations with various specialists.
Pre-Operative Assessments and Testing
Pre-operative assessments and testing are crucial in determining a patient’s candidacy for bone graft surgery and minimizing potential risks. The following medical tests and evaluations are commonly performed:
These evaluations help the surgical team determine the best approach for the patient and minimize the risk of complications.
Donor Bone Extraction or Preparation
The process of donor bone extraction or preparation varies depending on the type of bone graft being used and the patient’s individual needs.
For autografts, which involve using the patient’s own bone, the surgeon will typically harvest bone from an adjacent area or a distant site. This may involve a separate surgical procedure to extract the bone, which is then processed and prepared for grafting.
For allografts, which involve using donor bone from another person, the surgeon will typically obtain the bone from a tissue bank or a donor registry. The bone is then processed and sterilized before being implanted into the patient.
For demineralized bone matrix (DBM), which is a type of allograft, the surgeon will typically inject the DBM into the defect site. This promotes bone growth and regeneration.
Role of General Anesthesia and Post-Operative Pain Management
General anesthesia is often used in bone graft surgery to ensure the patient remains comfortable and pain-free during the procedure. The anesthesiologist will typically administer a combination of medications to induce general anesthesia, which may involve sedation, muscle relaxation, and pain relief.
After the surgery, the patient will typically experience some discomfort, numbness, or tingling in the affected area. The surgeon will often prescribe pain medications or other medications to manage these symptoms and promote healing.
It is essential for patients to follow the post-operative instructions provided by their surgeon, which may include rest, medication, and follow-up appointments to ensure proper healing and prevent complications.
The patient’s overall health and physical condition will significantly impact the success of the bone graft surgery. It is crucial for patients to follow the pre-operative and post-operative instructions carefully to ensure the best possible outcome.
The Bone Grafting Procedure
Bone grafting is a complex surgical procedure that involves transferring bone tissue from one part of the body to another to repair or rebuild damaged or diseased bone. The procedure requires meticulous planning, precise execution, and the use of specialized instruments and tools. In this section, we will delve into the different techniques used for bone grafting and the role of surgical instruments in the process.
Open vs. Minimally Invasive Approaches
Two primary approaches are used in bone grafting: open and minimally invasive. The choice of approach depends on the location and extent of the bone defect, as well as the patient’s overall health and medical history.
Surgical Instruments and Specialized Tools
The success of bone grafting surgery relies heavily on the use of specialized instruments and tools. These instruments are designed to precisely manipulate and shape the bone tissue, ensuring accurate placement and fixation of the graft.
Step-by-Step Diagram of the Bone Grafting Process, Bone grafts near me
The surgeon harvests bone tissue from the donor site using specialized instruments and tools.
The surgeon cleans and prepares the recipient site by removing any debris or damaged tissue.
The surgeon gently places the bone graft in the prepared recipient site, taking care to align it properly.
The surgeon secures the bone graft in place using specialized instruments and tools, ensuring proper fixation and stabilization.
Factors Influencing Bone Graft Success Rates and Outcomes

Bone graft success rates and outcomes can be influenced by a combination of factors, including patient age, bone quality, and overall health. These factors can impact the healing process and the long-term success of the bone graft. A comprehensive understanding of these factors is essential for surgeons and patients to make informed decisions about bone graft surgery.
Impact of Patient Age
Patient age is a crucial factor in bone graft success rates. Younger patients tend to have better bone quality and a faster healing process compared to older patients. As people age, bone density and quality decrease, making it more challenging for bone grafts to take hold. This can lead to a higher risk of complications and a lower success rate. Surgeons may consider age as a contraindication in certain cases.
Effect of Bone Quality
Bone quality is another critical factor in bone graft success rates. Patients with good bone quality tend to have a better outcome compared to those with poor bone quality. Bone quality can be affected by various factors, including genetics, lifestyle, and overall health. Patients with poor bone quality may require additional procedures or treatments to ensure the success of the bone graft.
| Bone Quality | Description |
|---|---|
| Good | Tight, dense, and well-structured bones |
| Poor | Lack of density, structure, or support |
Impact of Smoking
Smoking can have a significant impact on bone graft success rates. Chemicals in tobacco smoke can interfere with the healing process, leading to delayed recovery and an increased risk of complications. Surgeons often recommend that patients quit smoking before undergoing bone graft surgery.
Effect of Nutrition
Nutrition plays a vital role in bone healing and the success of bone grafts. Patients with a balanced diet rich in essential nutrients, such as calcium and vitamin D, tend to have a better outcome compared to those with poor nutrition. Surgeons often recommend a pre- and post-operative diet plan to ensure optimal nutrient intake.
Interactions Between Factors
The interactions between these factors can make it challenging to predict bone graft success rates. A decision tree diagram can help illustrate these interactions.
“Decision Tree Diagram:
Patient Age → Bone Quality → Smoking → Nutrition → Bone Graft Success Rate”
This diagram shows the potential interactions between patient age, bone quality, smoking, nutrition, and bone graft success rates. Surgeons can use this diagram as a tool to help patients understand the complex factors that influence bone graft success rates.
Final Conclusion: Bone Grafts Near Me
By choosing bone grafts near me, patients can take the first step towards a life free from pain and limited mobility. With our expertise and state-of-the-art technology, you can trust that you’re in good hands. Remember, bone grafts are just one option in a wider range of treatment options available to you.
Detailed FAQs
What are the different types of bone grafts available?
Bone grafts can be classified into four main categories: autologous, allogenic, xenogenic, and synthetic. Autologous bone grafts use the patient’s own bone tissue, while allogenic grafts come from another person. Xenogenic grafts are derived from animals, and synthetic grafts are made from synthetic materials.
What are the risks associated with bone graft surgery?
Like any surgical procedure, bone graft surgery carries certain risks and complications. These may include infection, nerve damage, and bleeding. Our experienced surgeons take every precaution to minimize these risks and ensure a smooth recovery.
How long does it take to fully recover from bone graft surgery?
The recovery time for bone graft surgery varies depending on the individual patient and the type of procedure undertaken. Generally, patients can expect to spend several weeks to several months recovering from surgery, during which time they may need to follow a rehabilitation program.
Are bone grafts near me suitable for everyone?
While bone grafts near me are a highly effective treatment option, they may not be suitable for everyone. Patients who are at risk of not healing properly, such as those with poor bone quality or certain medical conditions, may need to consider alternative options.