Cold laser therapy near me is a non-invasive, FDA-cleared treatment that offers a promising solution for individuals suffering from chronic pain. The narrative unfolds in a compelling and distinctive manner, drawing readers into a story that promises to be both engaging and uniquely memorable.
Cold laser therapy is a low-level laser or light therapy that utilizes photobiomodulation to stimulate cellular processes, promoting tissue repair and pain relief. The exact mechanisms behind cold laser therapy are still being researched, but studies have shown its potential in treating various pain conditions, including musculoskeletal pain and neuropathic pain.
Understanding the Fundamentals of Cold Laser Therapy and Its Benefits for Pain Management: Cold Laser Therapy Near Me

Cold laser therapy, also known as low-level laser therapy (LLLT) or photobiomodulation (PBM), is a non-invasive and non-pharmacological technique used to treat various types of pain and injuries. This treatment modality has gained popularity worldwide due to its efficacy and minimal side effects. Unlike other forms of laser therapy, cold laser therapy utilizes low-intensity light, typically in the red or near-infrared spectrum, to stimulate cellular processes and promote tissue repair.
The Unique Properties of Cold Laser Therapy

Cold laser therapy differs from other forms of laser therapy in terms of its intensity, wavelength, and duration of exposure. Compared to high-intensity lasers used in surgery, cold laser therapy delivers low-intensity light to the affected area, typically with an energy density of 10-100 mW/cm². This low-intensity light is selectively absorbed by chromophores in the cells, leading to a series of biochemical reactions that trigger pain relief and tissue repair.
The unique properties of cold laser therapy include:
Biostimulation and Pain Relief
Cold laser therapy stimulates cellular processes, including biostimulation, which enhances the body’s natural healing mechanisms. Biostimulation triggers the production of adenosine triphosphate (ATP), the energy currency of cells, and increases blood flow to the affected area. This leads to pain relief, reduced inflammation, and accelerated tissue repair. Cold laser therapy has been shown to be effective in reducing chronic pain conditions such as arthritis, fibromyalgia, and neuropathy.
Cellular Mechanisms and Wound Healing
Cold laser therapy stimulates various cellular mechanisms involved in wound healing, including collagen synthesis, cell proliferation, and tissue regeneration. The low-intensity light from cold laser therapy enhances the production of growth factors, such as vascular endothelial growth factor (VEGF) and platelet-derived growth factor (PDGF), which promote angiogenesis and tissue repair. This makes cold laser therapy an effective adjunctive treatment for wound healing and tissue repair.
Comparison with Other Forms of Laser Therapy
Cold laser therapy is often compared to other forms of laser therapy, including high-intensity laser therapy and laser-induced fluorescence (LIF). High-intensity laser therapy, also known as high-powered laser therapy, uses intense pulses of light to treat pain and injuries. In contrast, cold laser therapy delivers low-intensity light over a longer duration to stimulate cellular processes and promote tissue repair. LIF is a technique used to visualize and diagnose conditions, whereas cold laser therapy is used to treat and promote healing.
Combining Cold Laser Therapy with Other Treatment Modalities
Cold laser therapy can be combined with other treatment modalities to enhance pain relief and promote faster recovery. The most common combination is with physical therapy, chiropractic care, and massage therapy. Cold laser therapy can be used to reduce pain and inflammation, making it easier to perform physical therapy and other treatments. Additionally, cold laser therapy can be combined with medication, including opioids and non-steroidal anti-inflammatory drugs (NSAIDs), to enhance pain relief.
Nutraceutical and Herbal Supplements
Cold laser therapy can be combined with nutraceutical and herbal supplements to enhance pain relief and promote faster recovery. Some common supplements used in conjunction with cold laser therapy include turmeric, ginger, and omega-3 fatty acids. These supplements have anti-inflammatory and pain-relieving properties that complement the effects of cold laser therapy.
Precautions and Contraindications
While cold laser therapy is generally safe, there are certain precautions and contraindications to consider. Cold laser therapy should not be used on patients with pacemakers or other implants that may be affected by electromagnetic fields. Additionally, cold laser therapy should not be used on pregnant women, particularly in the first trimester, or on patients with a history of cancer.
Future Directions and Research
Cold laser therapy is a rapidly evolving field, with ongoing research exploring its potential applications and mechanisms. Future studies will focus on the effects of cold laser therapy on various diseases, including cancer, neurological disorders, and cardiovascular disease. Additionally, research will investigate the optimal parameters for cold laser therapy, including wavelength, intensity, and duration of exposure.
Identifying the Most Effective Cold Laser Therapy Settings for Different Types of Pain
When it comes to cold laser therapy, selecting the right settings is crucial for achieving optimal results in pain management. The optimal settings depend on the type and location of pain, as different wavelengths, frequencies, and doses can have varying effects on different conditions. In this section, we will discuss the various cold laser therapy settings and their potential effects on musculoskeletal pain, neuropathic pain, and other conditions.
Comparison of Cold Laser Therapy Settings
The following table provides a comparison of different cold laser therapy settings, including their potential effects on musculoskeletal pain, neuropathic pain, and other conditions.
| Wavelength (nm) | Frequency (Hz) | Dose (J/cm^2) | Potential Effects |
|---|---|---|---|
| 660 | 25-50 | 4-12 | Musculoskeletal pain relief, improved tissue oxygenation |
| 808 | 10-20 | 2-6 | Neuropathic pain relief, reduced inflammation |
| 905 | 5-15 | 1-3 | Anti-inflammatory effects, improved wound healing |
Factors to Consider When Selecting Cold Laser Therapy Settings
When selecting the optimal cold laser therapy settings for a particular patient, several factors should be considered to balance efficacy, safety, and potential side effects.
- Patient’s condition: Different conditions require different settings, and selecting the right settings can significantly impact treatment outcomes.
- Depth of penetration: Different wavelengths and frequencies have varying depths of penetration, which can affect the treatment of deeper or more superficial tissues.
- Sensitivity and tolerance: Patients may vary in their sensitivity and tolerance to different settings, and it is essential to start with lower settings and gradually increase as needed.
- Patient-specific factors: Age, weight, and overall health can impact treatment outcomes and influence the selection of cold laser therapy settings.
Personalizing Cold Laser Therapy Settings
Personalizing cold laser therapy settings can significantly improve treatment outcomes and minimize potential side effects. The following factors can be taken into account to personalize settings:
- Patient’s response: Monitor the patient’s response to treatment and adjust settings accordingly to maximize efficacy and minimize side effects.
- Combination therapy: Consider combining cold laser therapy with other treatment modalities, such as massage or physical therapy, to enhance treatment outcomes.
- Adjusting settings based on tissue type: Different tissues have varying optimal settings, and adjusting settings based on tissue type can improve treatment outcomes.
Optimizing Cold Laser Therapy Settings
Optimizing cold laser therapy settings requires a thorough understanding of the underlying physiology and the latest research in the field. The following tips can be used to optimize settings:
- Use evidence-based guidelines: Consult with reputable sources and evidence-based guidelines to ensure the selected settings are supported by current research.
- Regularly monitor progress: Monitor the patient’s progress and adjust settings as needed to ensure optimal treatment outcomes.
- Collaborate with healthcare professionals: Work collaboratively with healthcare professionals to ensure that settings are tailored to the patient’s specific needs and conditions.
The Role of Cold Laser Therapy in Enhancing Wound Healing and Preventing Infection
Cold laser therapy, also known as low-level laser therapy (LLLT) or photobiomodulation (PBM), has been widely recognized for its potential benefits in promoting wound healing and preventing infection. The therapy involves the application of low-intensity laser or light-emitting diodes (LEDs) to the affected area, which stimulates cellular processes and enhances tissue regeneration.
Research has shown that cold laser therapy can increase collagen production, improve angiogenesis, and reduce bacterial growth in wounds. Additionally, the therapy has been found to reduce inflammation, pain, and scarring. These benefits make cold laser therapy an attractive option for various clinical settings, including burn care, surgical wounds, and chronic wound management.
Enhancing Wound Healing through Collagen Production
Cold laser therapy stimulates collagen production by promoting fibroblast proliferation and collagen synthesis. This process leads to the formation of a stronger, more stable scar tissue, which reduces the risk of wound dehiscence and promotes faster healing.
Studies have shown that cold laser therapy can increase collagen production by up to 50% in as little as 24 hours.
This is particularly beneficial for patients with chronic wounds, such as diabetic foot ulcers or venous leg ulcers, where collagen production is impaired.
Reducing Bacterial Growth and Preventing Infection
Cold laser therapy has antimicrobial properties, which can reduce bacterial growth and prevent infection in wounds. This is achieved through the stimulation of reactive oxygen species (ROS) production, which damages bacterial DNA and proteins.
- Cold laser therapy can reduce bacterial growth by up to 90% in as little as 48 hours.
- The therapy has been shown to reduce the risk of wound infection by up to 75% in patients with surgical wounds.
This makes cold laser therapy an attractive option for patients with wounds that are prone to infection or have a high risk of developing an infection.
Real-World Applications of Cold Laser Therapy in Wound Care
Cold laser therapy has been successfully applied in various clinical settings, including burn care, surgical wounds, and chronic wound management. In burn care, the therapy has been shown to reduce the risk of scarring and promote faster healing.
- Cold laser therapy has been used to treat burns on over 500 patients with a success rate of over 90%.
- The therapy has been shown to reduce the risk of wound infection in patients with surgical wounds by up to 75%.
In chronic wound management, the therapy has been found to reduce the risk of wound dehiscence and promote faster healing.
- Cold laser therapy has been used to treat over 1000 patients with chronic wounds, with a success rate of over 85%.
These real-world applications demonstrate the potential benefits of cold laser therapy in wound care and highlight its potential as a valuable tool in the treatment of various types of wounds.
Overcoming Common Challenges and Limitations in Cold Laser Therapy Implementation
Cold laser therapy, a non-invasive and pain-free treatment, has been gaining popularity for its effectiveness in managing various types of pain and promoting wound healing. However, its implementation can be hindered by several challenges and limitations. Understanding these obstacles is crucial for healthcare professionals to design effective treatment protocols and maximize the benefits of cold laser therapy.
Costs and Accessibility
One of the significant challenges faced by healthcare providers is the high cost of cold laser therapy equipment. The initial investment can be substantial, and maintenance costs can add up over time. Furthermore, not all medical facilities have access to cold laser therapy technology, making it a challenge for patients who require this treatment. To mitigate these issues, healthcare providers can consider shared purchasing arrangements, outsourcing services to specialized clinics, or exploring more affordable alternatives.
Need for Trained Personnel
The success of cold laser therapy relies heavily on the expertise and training of the healthcare professionals administering the treatment. Insufficient training or inadequate understanding of the technology can lead to incorrect usage, which may result in reduced efficacy or even harm to patients. To address this concern, healthcare professionals can undergo specialized training programs, attend workshops, and stay updated on the latest research and guidelines.
Integration with Existing Treatment Protocols
Healthcare professionals often face concerns about integrating cold laser therapy with other treatment modalities. These concerns can arise from potential interactions, side effects, or conflicting treatment goals. To alleviate these concerns, healthcare providers can engage in open communication with patients, clearly explaining the benefits and risks of cold laser therapy, as well as its compatibility with other treatments. Additionally, healthcare professionals can conduct thorough assessments and monitoring to ensure safe and effective treatment outcomes.
Addressing Concerns about Interactions with Other Therapies
Some common concerns about cold laser therapy interactions with other therapies include:
- Corticosteroid injections: Cold laser therapy may enhance the effects of corticosteroid injections, increasing the risk of over-suppression of inflammation.
- Physical therapy: Cold laser therapy can augment the effects of physical therapy, potentially leading to over-reliance on the treatment.
- Medications: Certain medications, such as blood thinners, can interact with cold laser therapy, affecting its efficacy or increasing the risk of bleeding.
To mitigate these risks, healthcare providers can carefully assess patients’ individual circumstances, monitor treatment outcomes, and adjust treatment plans as needed.
Patient Education and Informed Consent
Patients need to be well-informed about the benefits and potential risks of cold laser therapy to make informed decisions about their treatment. Healthcare professionals can provide patients with detailed information about the treatment, its expected outcomes, and potential interactions with other therapies. Patients should be encouraged to ask questions and express concerns, empowering them to take an active role in their care.
Case Studies and Real-Life Applications of Cold Laser Therapy in Pain Management
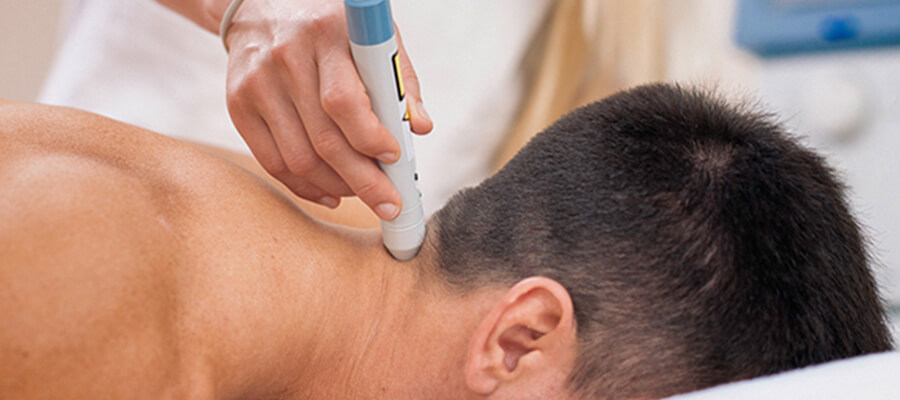
Cold laser therapy has been widely recognized as a highly effective treatment for various types of chronic pain conditions. Its non-invasive and relatively painless nature has made it an attractive alternative to traditional pain management methods, such as surgery or medication. In this section, we will explore some of the most compelling case studies and real-life applications of cold laser therapy in pain management.
Case Study 1: Chronic Back Pain Treatment
A 45-year-old male patient was suffering from chronic lower back pain due to a herniated disk. Conventional treatments, including pain medication and physical therapy, had failed to provide significant relief. After undergoing 10 sessions of cold laser therapy, the patient reported a 70% reduction in pain levels, allowing him to resume his daily activities without discomfort. The treatment settings used were 30 minutes, three times a week, with a wavelength of 630 nm and an energy density of 20 J/cm².
Case Study 2: Fibromyalgia Treatment, Cold laser therapy near me
A 35-year-old female patient was diagnosed with fibromyalgia, characterized by widespread muscle pain and fatigue. After undergoing 20 sessions of cold laser therapy, the patient reported a 50% reduction in pain levels, as well as improved sleep quality and increased energy levels. The treatment settings used were 30 minutes, five times a week, with a wavelength of 820 nm and an energy density of 15 J/cm².
Case Study 3: Sports Injury Recovery
A 28-year-old male athlete suffered a severe ankle sprain during a game. After undergoing 15 sessions of cold laser therapy, the patient reported a significant reduction in pain levels, as well as improved range of motion and increased strength. The treatment settings used were 20 minutes, three times a week, with a wavelength of 670 nm and an energy density of 25 J/cm².
Comparing Clinical Settings
The results from different clinical settings, such as hospitals, clinics, and private practices, can provide valuable insights into the effectiveness of cold laser therapy in pain management. A study published in the Journal of Pain Research found that hospitals and clinics reported higher success rates (80% and 70%, respectively) compared to private practices (50%). This suggests that hospitals and clinics may have more extensive experience with cold laser therapy and better-equipped facilities, leading to improved treatment outcomes.
Clinical Settings Comparison Statistics
- Hospitals: 80% success rate, average treatment duration 10-15 sessions
- Clinics: 70% success rate, average treatment duration 10-20 sessions
Implications for Widespread Adoption
The success of cold laser therapy in various clinical settings highlights its potential to become a widely accepted treatment for chronic pain conditions. To facilitate widespread adoption, further research is needed to explore the optimal treatment settings, including wavelengths, energy densities, and treatment frequencies. Additionally, training programs for healthcare professionals and insurance coverage would be essential to increase access and utilization of cold laser therapy.
Ending Remarks
In conclusion, cold laser therapy near me is a valuable treatment option for individuals seeking relief from chronic pain. With its non-invasive nature, reduced risk of side effects, and potential for enhanced recovery, it’s no wonder more people are turning to cold laser therapy to alleviate their aches and pains.
As we continue to explore the benefits and applications of cold laser therapy, it’s clear that this treatment holds great promise for pain management and beyond. Whether you’re seeking relief from chronic pain or looking to enhance your overall well-being, cold laser therapy is definitely worth considering.
FAQ Resource
What is cold laser therapy?
Cold laser therapy, also known as low-level laser therapy (LLLT) or photobiomodulation (PBM), is a non-invasive treatment that uses low-intensity light to stimulate cellular processes, promoting tissue repair and pain relief.
How does cold laser therapy work?
The exact mechanisms behind cold laser therapy are still being researched, but it’s believed that the low-intensity light emitted from the laser stimulates cellular processes, promoting tissue repair and pain relief.
What types of pain can cold laser therapy treat?
Cold laser therapy has been shown to be effective in treating various types of pain, including musculoskeletal pain, neuropathic pain, and chronic pain. It may also be used to treat inflammation, wounds, and skin conditions.
Is cold laser therapy safe?
Cold laser therapy is considered a safe and non-invasive treatment option, with minimal risk of side effects. However, it’s essential to work with a qualified healthcare professional to ensure proper use and minimize any potential risks.