With fungus nail doctor near me at the forefront, it’s time to take care of those pesky toenail infections that have been plaguing you for months. But did you know that fungal nail infections are more common than you think, and can be easily prevented with the right knowledge and attention? Let’s dive into the world of fungal nail infections and explore the best ways to treat and prevent them.
This comprehensive guide will walk you through the definition and types of fungal nail infections, the causes and triggers that make you susceptible, and the different diagnosis and treatment options available to you. We’ll also explore the importance of choosing the right fungus nail doctor near you, and share expert tips on how to prevent fungal nail infections from striking again.
Definition of Fungal Nail Infections
A fungal nail infection, also known as onychomycosis, is a common condition that affects the nails and is typically characterized by discoloration, thickening, and brittleness of the affected nail. It occurs when a fungus, such as Trichophyton, Candida, or Aspergillus, infects the nail plate, nail bed, or nail matrix. This infection can be quite painful and may lead to embarrassment due to the unpleasant appearance of the infected nail.
Fungal nail infections occur in conditions that allow the fungus to thrive, such as warm and moist environments, and poor foot hygiene. Individuals who engage in sports or activities that involve being in water for extended periods, such as swimmers, are at a higher risk of contracting these infections. People with weakened immune systems, diabetes, or circulatory problems are also more likely to suffer from fungal nail infections.
Places where people can contract fungal nail infections
People can contract fungal nail infections in various places, including:
-
Fungal nail infections can be contracted from public pools, lakes, or oceans where the fungus thrives in warm and moist environments. In order to contract the infection, one needs to have tiny cuts or cracks in the nail or on the surrounding skin. This provides an entry point for the fungus to attach and start the infection process.
- Onychomycosis: Onychomycosis is the most common type of fungal nail infection, accounting for about 50% of all fungal nail infections. It is characterized by thickening, discoloration, and brittleness of the nail plate. The infection usually starts at the tip of the nail and spreads to the rest of the nail plate.
- Distal Subungual Onychomycosis: This type of fungal nail infection is characterized by a yellow or white spot on the tip of the nail plate. The infection usually starts at the tip of the nail and spreads to the rest of the nail plate.
- Proximal Subungual Onychomycosis: This type of fungal nail infection is characterized by a yellow or white spot on the underside of the nail plate. The infection usually starts on the nail bed and spreads to the nail plate.
- Causes: Fungal nail infections can be caused by a variety of fungi, including Candida, Trichophyton, and Aspergillus. The fungi can infect the nail plate, nail bed, or surrounding tissue.
- Symptoms: The symptoms of fungal nail infections can include thickening, discoloration, and brittleness of the nail plate, as well as pain, itching, and inflammation of the nail bed and surrounding tissue.
- Topical Antifungal Agents: Topical antifungal agents can be applied directly to the nail plate or nail bed to treat fungal nail infections.
- Oral Antifungal Agents: Oral antifungal agents can be taken orally to treat fungal nail infections.
- Surgical Treatment: In severe cases of fungal nail infections, surgical treatment may be necessary to remove the infected nail and prevent further infection.
- Physical Examination: A physical examination of the nail plate and nail bed can help diagnose fungal nail infections.
- Nail Scraping: A nail scraping test can be performed to collect a sample of the infected nail plate or nail bed for laboratory analysis.
- Dermatophyte Test Medium (DTM) Culture: A DTM culture can be performed to confirm the diagnosis of fungal nail infections.
- Punch Biopsy: A punch biopsy can be performed to collect a sample of the infected nail plate or nail bed for laboratory analysis.
- Sweating excessively, especially during physical activity or in hot temperatures
- Sharing personal care items, such as nail clippers or files, or walking barefoot in public areas like communal showers or pools
- Wearing shoes that are too tight or don’t allow for airflow, creating a moist environment around the feet
- Not drying the feet thoroughly after bathing or showering
- Dysglycemia (blood sugar fluctuations) can weaken the immune system, making it harder for the body to fight off fungal infections
- Neuropathy can lead to poor circulation, causing nail growth to slow down and become more susceptible to fungal infections
- Soak your toes in a mixture of water and vinegar for 15-20 minutes, 2-3 times a week.
- Apply a small amount of tea tree oil or lavender oil directly to the affected area, 2-3 times a day.
- Keep your toenails dry and clean to prevent further infection and promote the healing process.
- A medical degree (MD) or a Doctor of Podiatric Medicine (DPM) degree.
- Board certification in a relevant medical field, such as dermatology or podiatry.
- Postgraduate training in fungal nail infections or a related field.
- Membership in professional organizations, such as the American Academy of Dermatology or the American Podiatric Medical Association.
- A good reputation among peers and patients, with positive online reviews and ratings.
-
Wash your feet twice a day with soap and warm water, paying special attention to the areas between your toes.
Dry your feet thoroughly after washing, especially between the toes.
Trim your toenails properly to avoid cutting the nails too short, which can lead to nail infections. -
Wear breathable footwear that allows for airflow, such as sandals or shoes with a mesh upper.
Change your socks regularly to prevent moisture buildup in your shoes.
Use an antifungal powder or spray on your feet to help prevent fungal growth. -
Disinfect your toenail clippers after each use with soap and water, and dry them thoroughly.
Don’t share personal care items with others to prevent the spread of infection.
Avoid walking barefoot in public areas where fungus may be present. -
Consult your doctor about any medications or treatments that may be contributing to your compromised immune system.
Practice regular foot hygiene as mentioned earlier.
Consider using antifungal medications or creams specifically designed to combat fungal infections. -
Keep your feet clean and dry at all times, paying special attention to areas between the toes.
Avoid sharing personal care items with others to prevent the spread of infection.
Get regular check-ups with your doctor to monitor your foot health.
Public showers or locker rooms where the fungus accumulates on the wet surfaces. The fungus can then easily infect the skin and nails, leading to painful and unsightly infections.
Nail salons where instruments are not properly sterilized. Using contaminated instruments can spread the fungus from one person to another, causing infections.
Fungal nail infections can also be contracted by sharing personal care items, such as nail clippers or files, without proper cleaning and disinfection.
High-risk population
The following population groups are at a high risk of contracting fungal nail infections:
-
Individuals with diabetes, circulatory problems, or weakened immune systems are more prone to fungal nail infections. This is because their bodies are less able to fight off the infection, making them more susceptible.
Older adults are also at a higher risk of contracting fungal nail infections. As people age, their nail growth slows down, making it easier for the fungus to infect the nail.
Athletes or individuals who engage in sports that involve being in water for extended periods are at a higher risk of contracting fungal nail infections. This is because their feet are more likely to be exposed to warm and moist environments, providing an ideal environment for the fungus to grow.
Why fungal nail infections are hard to treat
Fungal nail infections are difficult to treat due to the following medical reasons:
-
The fungus that causes the infection, such as Trichophyton, Candida, or Aspergillus, is highly resistant to treatment. This makes it challenging to kill the fungus, leading to prolonged treatment periods.
The nail plate serves as a barrier, making it difficult for the fungus to penetrate and become visible. As a result, it can be challenging to diagnose the infection accurately, making treatment even more difficult.
Fungal nail infections often require prolonged treatment, which can be frustrating for patients. This is because the infection may take several months to a year or more to resolve, depending on the severity and location of the infection.
Types of Fungal Nail Infections
Fungal nail infections are caused by a variety of fungi that infect the nail plate, nail bed, or surrounding tissue. These infections can range from mild to severe and may be difficult to treat. There are several types of fungal nail infections, each with its unique characteristics, symptoms, and treatment options.
Common Types of Fungal Nail Infections
Fungal nail infections can be broadly categorized into several types based on their symptoms, causes, and treatment options. The following are the most common types of fungal nail infections:
Causes and Symptoms of Fungal Nail Infections
Fungal nail infections are caused by a variety of fungi that thrive in warm, moist environments. The causes and symptoms of fungal nail infections can vary depending on the type of infection. The following are some common causes and symptoms of fungal nail infections:
Treatment Options for Fungal Nail Infections
Fungal nail infections can be treated with a variety of medications, including topical and oral antifungal agents. The following are some common treatment options for fungal nail infections:
Methods for Diagnosing Fungal Nail Infections
Diagnosing fungal nail infections can be challenging, but several methods can be used to confirm the diagnosis. The following are some common methods for diagnosing fungal nail infections:
Table: Types of Fungal Nail Infections
| Types of Infections | Common Symptoms | Treatment Options | Preventative Measures |
|---|---|---|---|
| Onychomycosis | Thickening, discoloration, and brittleness of the nail plate | Topical and oral antifungal agents, surgical treatment | Wear shoes and socks made of breathable materials, dry feet and toes thoroughly, avoid sharing personal care items |
| Distal Subungual Onychomycosis | Yellow or white spot on the tip of the nail plate | Topical and oral antifungal agents, surgical treatment | Wear shoes and socks made of breathable materials, dry feet and toes thoroughly, avoid sharing personal care items |
| Proximal Subungual Onychomycosis | Yellow or white spot on the underside of the nail plate | Topical and oral antifungal agents, surgical treatment | Wear shoes and socks made of breathable materials, dry feet and toes thoroughly, avoid sharing personal care items |
Causes and Triggers of Fungal Nail Infections
Fungal nail infections can be caused by a combination of factors, including poor foot hygiene, exposure to fungal spores, and underlying medical conditions. When it comes to fungal nail infections, it’s essential to understand the causes and triggers to take preventive measures.
The Role of Moisture and Poor Foot Hygiene
—————————————-
Moisture and poor foot hygiene are significant contributors to fungal nail infections. When the feet are exposed to excessive moisture, it creates an ideal environment for fungal growth. This can occur in various situations, such as:
These situations can lead to the proliferation of fungal spores, which can then infect the nail bed.
Factors that Increase the Risk of Fungal Nail Infections in People with Diabetes
Diabetes can increase the risk of fungal nail infections due to several factors. People with diabetes are more prone to developing diabetic foot ulcers, which can lead to fungal infections. Additionally, diabetes-related conditions like neuropathy can cause nerve damage, leading to poor circulation and increased susceptibility to fungal infections.
The Relationship between Foot Temperature, Humidity, and Fungal Growth
Temperature and humidity play a significant role in the growth and proliferation of fungi.
The optimal temperature for fungal growth is between 68°F and 82°F (20°C and 28°C), with a relative humidity of 70-80%. At these temperatures and humidity levels, fungi can grow rapidly.
| Temperature (°F) | Humidity (%) | Fungal Growth |
|---|---|---|
| 20-28°C | 70-80% | Average to High |
| Below 20°C or above 28°C | Below 50% or above 80% | Minimal to Low |
Diagnosis and Treatment of Fungal Nail Infections: Fungus Nail Doctor Near Me

Diagnosing fungal nail infections can be a challenging process, as the symptoms may resemble those of other conditions, such as nail trauma or nutritional deficiencies. However, with the right medical tests and tools, a correct diagnosis can be made, allowing for effective treatment to begin.
Diagnosing Fungal Nail Infections
The diagnosis of fungal nail infections typically involves a combination of medical history, physical examination, and laboratory tests. Your doctor may ask you questions about your symptoms, medical history, and lifestyle habits to understand the severity of the infection. A physical examination of your nail will help your doctor to visualize the infection and determine the extent of damage.
During the physical examination, your doctor may perform the following tests:
* Scrape test: A small sample of cells from the affected area is taken and examined under a microscope for fungal hyphae (branching filaments).
* Wood’s lamp test: A special light is used to examine the affected area for the presence of fungal spores.
* Nail clippings: A sample of nail clippings is taken and sent to a laboratory for culture and examination.
In addition to these tests, your doctor may also recommend the following:
* Fungal culture: A sample of nail clippings or tissue is taken and cultured to identify the type of fungus causing the infection.
* Blood tests: To rule out underlying conditions, such as autoimmune disorders or nutritional deficiencies.
Treatment Options for Fungal Nail Infections
The treatment for fungal nail infections depends on the severity and location of the infection, as well as the individual’s overall health. Mild cases of fungal nail infections may be treated with topical creams or ointments, while more severe cases may require oral medications.
The following are some common treatment options for fungal nail infections:
* Topical creams and ointments: Apply directly to the affected area, these creams and ointments can help to reduce symptoms and slow the progression of the infection.
* Oral medications: Taken by mouth, these medications can help to kill the fungus and promote the growth of healthy nail tissue.
* Laser treatment: A high-energy beam is used to target and destroy the fungal hyphae, which can help to clear the infection.
* Home remedies: While not as effective as medical treatments, home remedies such as tea tree oil, lavender oil, and vinegar may help to promote the healing process and prevent further infection.
Home Remedies for Fungal Nail Infections, Fungus nail doctor near me
While not a replacement for medical treatment, home remedies can help to promote the healing process and prevent further infection. Some of the most effective home remedies include:
* Tea tree oil: A natural antifungal agent, tea tree oil can be applied directly to the affected area to help clear the infection.
* Lavender oil: Antifungal and antibacterial properties make lavender oil a great option for promoting healing and preventing infection.
* Vinegar: Soaking the affected toe in a mixture of water and vinegar can help to reduce the pH level and prevent further infection.
Keep in mind that home remedies may not be as effective as medical treatments, and it’s always best to consult with a doctor before attempting to treat fungal nail infections at home.
Choosing the Right Fungus Nail Doctor Near Me
When it comes to treating fungal nail infections, choosing the right doctor is crucial for effective treatment and a speedy recovery. With numerous options available, it can be overwhelming to decide which doctor to consult. In this section, we will guide you on how to choose the right fungus nail doctor near you.
Qualifications and Experience of Fungus Nail Doctors
When selecting a doctor to treat your fungal nail infection, it is essential to consider their qualifications and experience in the field. A doctor specializing in fungal nail infections should have extensive knowledge and experience in diagnosing and treating various types of fungal infections. They should have a strong understanding of the different causative agents, treatment options, and potential complications associated with fungal nail infections.
To evaluate a doctor’s qualifications, look for:
Importance of Consulting a Doctor Before Self-Diagnosing and Treating Fungal Nail Infections
Self-diagnosing and treating fungal nail infections can lead to inaccurate diagnoses, delayed treatment, and potential complications. Consulting a doctor experienced in fungal nail infections ensures that you receive an accurate diagnosis and tailored treatment plan. A doctor can also provide guidance on how to prevent future infections and manage related symptoms.
Consulting a doctor before treating your fungal nail infection is crucial because:
* They can perform a thorough examination and take a thorough medical history to determine the cause of your symptoms.
* They can prescribe effective treatment options, such as topical or oral antifungal medications, and recommend lifestyle changes to prevent future infections.
* They can monitor your progress and adjust your treatment plan as needed.
* They can detect potential complications, such as toenail fungus, and provide guidance on how to manage them.
Characteristics of an Ideal Fungus Nail Doctor
When selecting a fungus nail doctor, consider the following characteristics to ensure that you receive quality care:
* Bedside manner: A good doctor should be compassionate, empathetic, and communicative, making you feel heard and understood.
* Expertise: A doctor with extensive knowledge and experience in fungal nail infections is more likely to provide effective treatment and guidance.
* Office hours: A doctor with convenient office hours, including evenings and weekends, can accommodate your schedule and provide flexibility.
* Availability: A doctor with a quick response time and minimal wait time can ensure that you receive timely care.
An ideal fungus nail doctor should possess a combination of technical expertise, bedside manner, and accessibility. They should be able to provide comprehensive care, including diagnosis, treatment, and prevention, while making you feel comfortable and confident in their abilities.
Preventing Fungal Nail Infections: Importance of Foot Hygiene
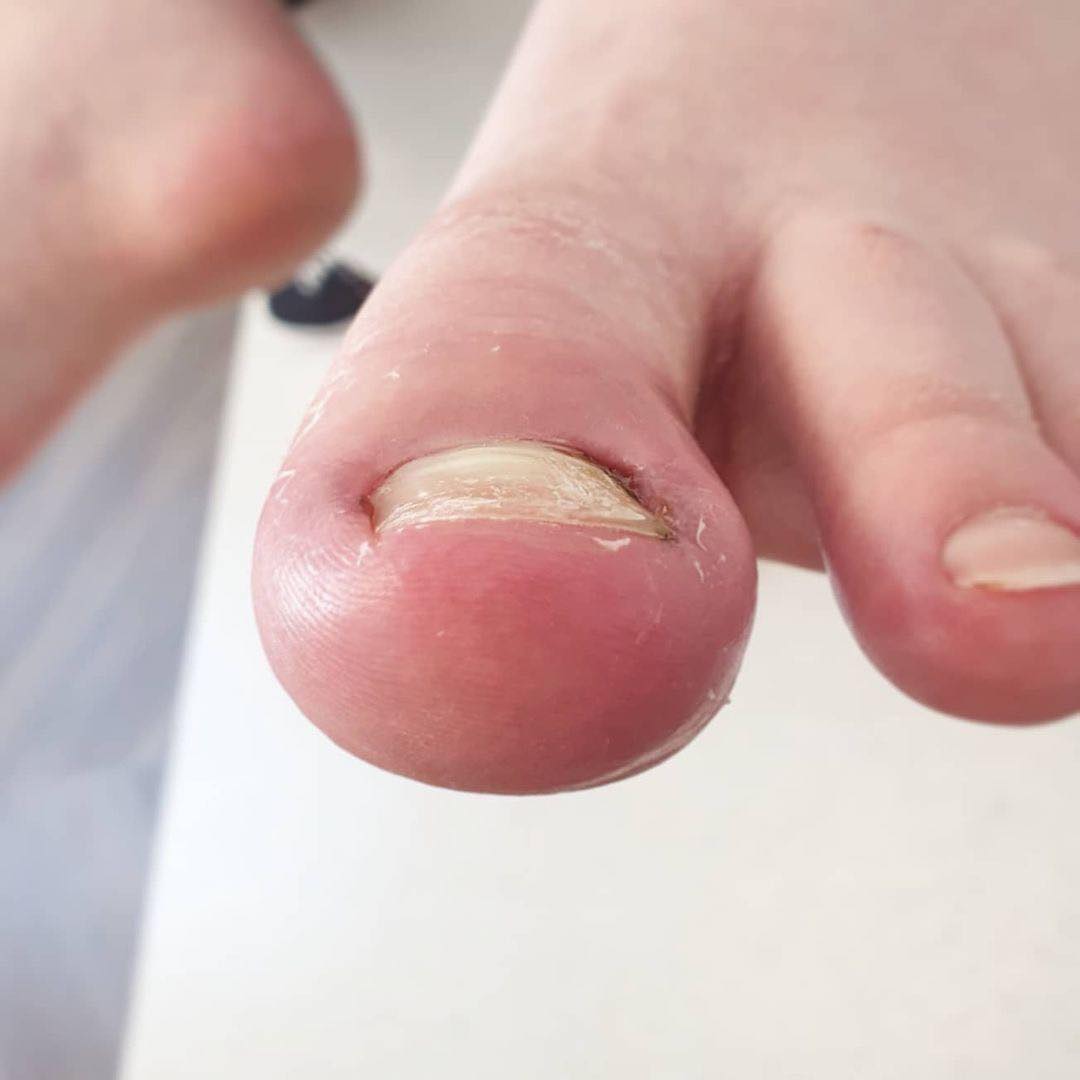
Maintaining proper foot hygiene is crucial in preventing fungal nail infections. These infections can spread quickly when the feet sweat excessively or come into contact with contaminated surfaces. Proper foot hygiene can help prevent the growth and spread of fungi, reducing the risk of infection.
Key Steps to Improve Foot Hygiene
To maintain proper foot hygiene, follow these steps:
Reducing Risk in People with Compromised Immune Systems
Individuals with compromised immune systems are more susceptible to fungal nail infections. To reduce the risk of infection, follow these additional steps:
Benefits of Prevention
Preventing fungal nail infections is generally more effective than treating them once they occur. The early signs of a fungal infection may be subtle, but prompt treatment is necessary to prevent further damage and potential complications.
Conclusive Thoughts
So, the next time you notice a discolored or thickened toenail, don’t hesitate to reach out to a trusted fungus nail doctor near you. With the right treatment and prevention strategies, you can regain healthy, strong, and beautiful nails that exude confidence and style. Remember, a healthy nail is just a visit away!
Clarifying Questions
Q: What causes fungal nail infections?
Fungal nail infections occur when tiny fungi that are normally present on the skin and nails overgrow and infect the nail bed. Moisture, poor foot hygiene, and weakened immune systems are all contributing factors.
Q: How do I choose the right fungus nail doctor near me?
When selecting a fungus nail doctor near you, look for professionals with extensive experience in treating fungal nail infections, a clean and hygienic clinic, and a compassionate bedside manner.
Q: Can I treat fungal nail infections at home?
While home remedies can provide temporary relief, they are not a substitute for professional medical treatment. Consult a fungus nail doctor near you for accurate diagnosis and effective treatment options.
Q: How can I prevent fungal nail infections?
Preventing fungal nail infections is easier than you think! Practice good foot hygiene, wear clean socks, dry your feet thoroughly, and avoid sharing personal care items to reduce the risk of fungal nail infections.