Diabetic pedicure near me is a must-have for those with sensitive feet, especially when living in a crowded city like Jakarta. The risks of complications and infections are ever-present, but a well-planned diabetic pedicure can reduce these risks and promote overall foot health. But have you ever wondered what a customized diabetic pedicure entails? In this article, we’ll dive into the world of diabetic pedicure near me and explore the specific needs of individuals with diabetes who experience sensitive feet.
A diabetic pedicure is more than just a routine foot care procedure. It’s a specialized approach that requires podiatrists or trained medical professionals to provide guidance on foot care for those with diabetes. The process involves assessing a client’s foot, identifying areas where the skin may be more prone to irritation or pressure, and selecting the right materials for the pedicure, considering any allergies or sensitivities the client may have.
Understanding the Importance of Customized Diabetic Pedicures for Sensitive Feet: Diabetic Pedicure Near Me
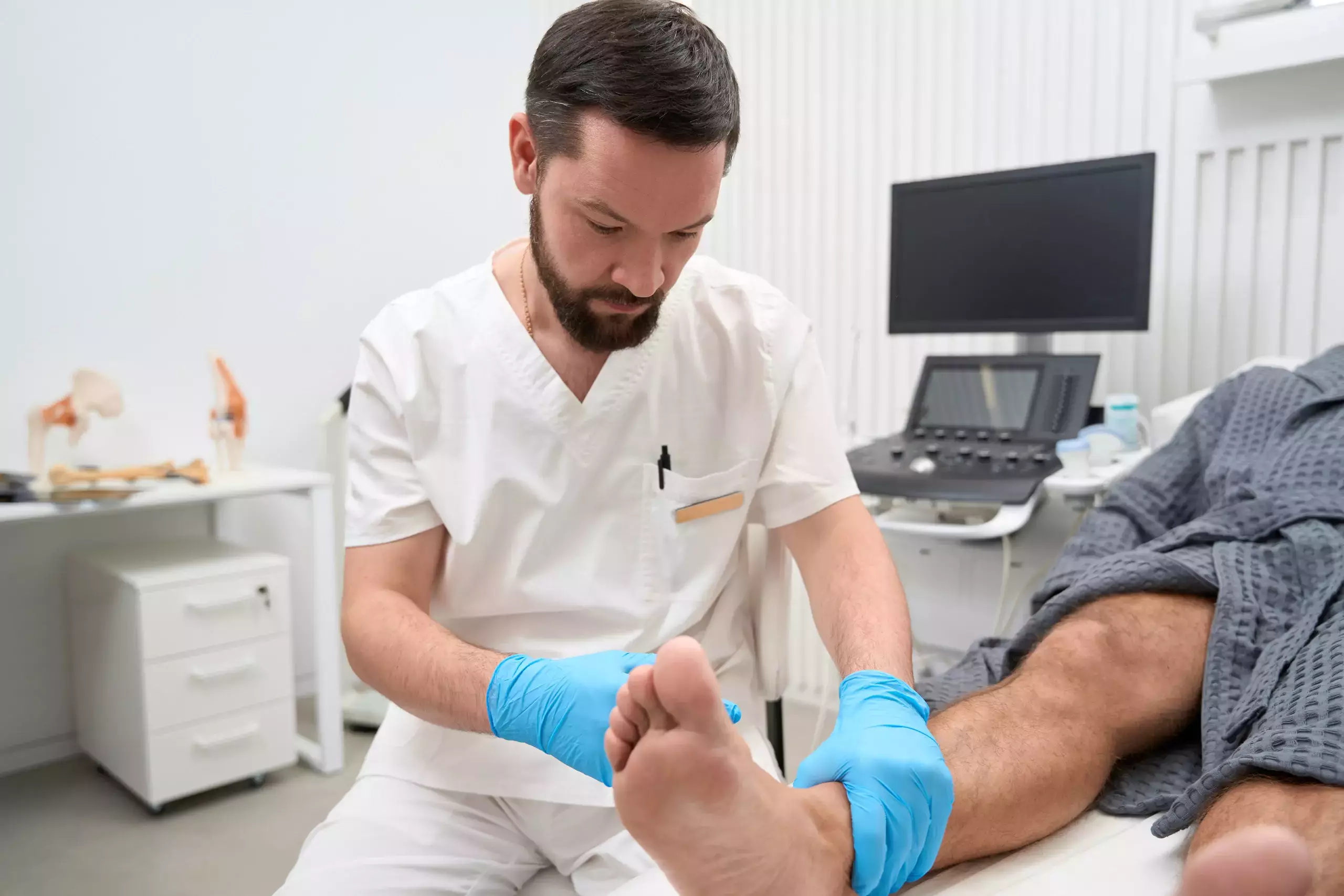
Individuals with diabetes often face a multitude of challenges related to their foot health. One of the most pressing concerns for those with diabetes is the sensitivity and fragility of their feet. Sensitive feet can be a sign of underlying complications, such as nerve damage (neuropathy) or poor blood circulation, which can increase the risk of infections and ulcers. In fact, the American Diabetes Association estimates that approximately 60% of all lower-limb amputations in the United States occur among individuals with diabetes, with many of these procedures resulting from untreated foot ulcers.
For those with sensitive feet, it is essential to adopt a customized approach to foot care, one that prioritizes prevention, early detection, and regular maintenance. This is where a well-planned diabetic pedicure comes into play. A diabetic pedicure is a specialized foot care treatment designed to address the unique needs of individuals with diabetes. This includes gentle exfoliation, meticulous nail care, and precise trimming to prevent ingrown toenails and other common problems associated with sensitive feet.
Risks Associated with Sensitive Feet
Sensitive feet are a warning sign of potential complications, including:
- Peripheral neuropathy, a condition in which the nerves that transmit pain and sensation signals to the brain are damaged, leading to decreased sensitivity and numbness in the feet.
- Poor blood circulation, which can cause swelling, discoloration, and slow healing of wounds.
- Infections, such as cellulitis or osteomyelitis, which can spread quickly through the bloodstream and cause severe complications.
- Foot ulcers, which can become infected and lead to amputation if left untreated.
These complications can have devastating consequences, including increased risk of hospitalization, disability, and even mortality.
The Role of Podiatrists in Diabetic Foot Care
Podiatrists, also known as foot doctors or chiropodists, play a vital role in the prevention and management of foot-related complications in individuals with diabetes. They are trained healthcare professionals who specialize in the diagnosis, treatment, and prevention of disorders and conditions of the foot and ankle.
When it comes to diabetic foot care, podiatrists can:
- Provide personalized foot care plans to address the unique needs of each patient.
- Conduct regular check-ups to detect early signs of complications, such as foot ulcers or infections.
- Offer expert advice on proper foot hygiene, shoe selection, and footwear care.
- Perform specialized treatments, including debridement, antibiotics, and orthotics, to help manage foot ulcers and prevent recurrence.
Establishing a Regular Foot Care Routine
For individuals with diabetes who have been diagnosed with peripheral neuropathy or are at risk of developing ulcers, establishing a regular foot care routine is crucial. This may involve:
- Regularly inspecting the feet for signs of cracks, cuts, or other wounds.
- Washing the feet daily with mild soap and lukewarm water.
- Using a pumice stone or foot file to gently exfoliate rough patches.
- Moisturizing the skin to prevent dryness and cracking.
- Wearing properly fitting shoes with good arch support and cushioning.
By following these guidelines and consulting with a podiatrist regularly, individuals with diabetes can reduce their risk of complications and maintain healthy, sensitive feet for years to come.
‘A well-planned diabetic pedicure can reduce the risk of complications, promote overall foot health, and improve the quality of life for individuals with diabetes.’
A Step-by-Step Guide to Customizing a Diabetic Pedicure

Customizing a diabetic pedicure requires a thorough understanding of the client’s foot anatomy, common foot pathologies, and the specific challenges faced by individuals with diabetes. The goal is to provide a safe and effective pedicure that minimizes the risk of infection and promotes healthy foot care.
Assessing the Foot
To customize a diabetic pedicure, it is essential to conduct a thorough assessment of the client’s foot. This involves inspecting the foot for any visible signs of irritation, pressure, or infection. The following parameters should be evaluated: circulation, sensation, and nail morphology.
–
Inspect the Foot for Visible Signs of Irritation or Pressure
When assessing the foot, look for any visible signs of irritation or pressure, such as redness, swelling, or thickening of the skin. Check for any areas of callus formation, where the skin may be more prone to irritation.
–
Check for Deformities or Abnormalities in the Foot’s Anatomy
Pay particular attention to any deformities or abnormalities in the foot’s anatomy, such as hammertoes or bunions. These can put pressure on specific areas of the foot, increasing the risk of irritation or infection.
Selecting the Right Materials
When selecting materials for the pedicure, consider any allergies or sensitivities the client may have. Use gentle, sterile instruments and choose products that are fragrance-free and hypoallergenic. If the client has a history of allergic reactions, use a patch test to ensure that the products do not cause an adverse reaction.
The Procedures Involved in Providing a Diabetic Pedicure
A diabetic pedicure involves the following procedures: debridement, nail shaping, and the application of moisturizers. These procedures are designed to promote healthy foot care and minimize the risk of infection.
Debridement
Debridement is the removal of dead or damaged tissue to promote healing and prevent infection. The following tools may be used for debridement:
–
Debridement Tools
– Urea paste
– Hydrogen peroxide
– Saline solution
Debridement tools may be used in various combinations to achieve optimal results:
- Apply a thick layer of urea paste to the affected area and let it sit for a few minutes before rinsing it off with a saline solution.
- Use hydrogen peroxide to break down dead tissue.
The rationale behind using debridement tools is to remove dead tissue that can harbor bacteria and lead to infection. By promoting the removal of dead tissue, debridement helps to prevent the development of pressure ulcers and reduces the risk of foot amputation.
Nail Shaping
Nail shaping is an essential part of a diabetic pedicure, as it helps to reduce the risk of ingrown toenails and other nail-related complications. Use a nail clipper or nail scissors to carefully trim the toenails, taking care to avoid cutting the nails too short.
Application of Moisturizers
After the pedicure, apply a moisturizer to the feet to keep the skin hydrated and supple. This is especially important for individuals with diabetes, as they are more prone to dry skin and foot infections.
- Apply a moisturizer to the feet after bathing, paying special attention to areas between the toes.
- Use a rich, hydrating moisturizer to keep the skin moisturized and prevent dryness.
The application of moisturizers is essential for maintaining healthy, hydrated skin, especially for individuals with diabetes. By keeping the skin hydrated, you can prevent dryness, cracking, and other complications that can lead to infection.
Special Considerations for Diabetic Patients Undergoing a Pedicure
Diabetic patients require special attention during a pedicure to ensure their foot health is not compromised. This includes considering medications, health conditions, and circulatory issues that may impact their foot health.
Modifying the Pedicure Process for Circulatory Issues
For individuals with circulatory issues, it is essential to ensure they receive adequate oxygenation to their feet. Circulatory issues can lead to swelling, bruising, or pain, which can be exacerbated by a pedicure. To modify the pedicure process, follow these guidelines:
- Begin by elevating the foot to reduce swelling and promote blood flow.
- Use gentle strokes and avoid massaging areas with poor circulation.
- Choose creams or lotions rich in emollients and humectants to help moisturize and soften the skin.
- Avoid using heat or harsh chemicals, as they can exacerbate circulatory issues.
- Monitor the individual’s temperature and adjust as needed to prevent overheating.
- Consider using a humidifier in the room to maintain a comfortable moisture level.
When providing adequate oxygenation, it is crucial to ensure the individual is comfortable and relaxed throughout the pedicure process. This can be achieved by:
- Creating a soothing atmosphere with calming music and a relaxing environment.
- Using gentle, soothing touch to reduce stress and anxiety.
- Encouraging the individual to breathe deeply and slowly, promoting relaxation.
- Using aromatherapy, such as lavender or chamomile, to promote relaxation and reduce stress.
By modifying the pedicure process and providing adequate oxygenation, individuals with circulatory issues can benefit from a safe and relaxing pedicure experience.
Adequate oxygenation is essential for wound healing and overall foot health. By ensuring the individual receives proper oxygenation, you can promote healing and reduce the risk of complications.
Monitor the individual’s temperature, heart rate, and overall comfort level throughout the pedicure process. If they experience any discomfort or pain, adjust the treatment accordingly.
Identifying and Addressing Signs of Infection
It is crucial to monitor for signs of infection during a pedicure, especially for diabetic patients. Infection can be a serious complication for individuals with diabetes, as it can lead to more severe health issues.
Medications and Health Conditions that May Impact Foot Health, Diabetic pedicure near me
Certain medications and health conditions can impact foot health, making it essential to consider these factors when performing a pedicure. Common medications that may impact foot health include:
- Narcotics, which can cause dizziness and disorientation.
- Antihistamines, which can dry out the skin and exacerbate circulatory issues.
- Blood thinners, which can increase the risk of bleeding and bruising.
Common health conditions that may impact foot health include:
- Diabetes, which can lead to nerve damage, circulatory issues, and foot ulcers.
- Kidney disease, which can lead to poor circulation and swelling.
- Autoimmune disorders, which can cause inflammation and pain.
By understanding these special considerations, you can provide a safe and relaxing pedicure experience for diabetic patients.
Final Thoughts

In conclusion, a diabetic pedicure near me is an essential part of maintaining healthy feet, especially for individuals with diabetes. By following the tips and guidelines Artikeld in this article, you can enjoy a safe and effective foot care experience. Don’t wait until it’s too late – take care of your feet today and reduce the risk of complications and infections.
Question & Answer Hub
Q: What is diabetic pedicure near me?
A: Diabetic pedicure near me is a specialized foot care procedure designed for individuals with diabetes who experience sensitive feet. It requires podiatrists or trained medical professionals to provide guidance on foot care to reduce the risk of complications and infections.
Q: What are the risks of complications and infections for individuals with diabetes who experience sensitive feet?
A: Individuals with diabetes who experience sensitive feet are at risk of developing ulcers, infections, and other complications. Regular foot care is essential to prevent these risks and promote overall foot health.
Q: Who should provide guidance on foot care for individuals with diabetes?
A: Podiatrists or trained medical professionals are the best individuals to provide guidance on foot care for individuals with diabetes. They can assess the client’s foot, identify areas of concern, and provide personalized recommendations for foot care.
Q: What are some tips for maintaining healthy feet as a diabetic?
A: Regularly cleaning and disinfecting the feet, removing calluses and dead skin, and protecting the skin from excessive moisture are crucial for maintaining healthy feet as a diabetic. Additionally, regular foot care check-ups with a podiatrist or trained medical professional can help identify potential issues before they become serious.